Business Knowledge Guide
In a world where mental health and substance abuse challenges are increasingly coming to the forefront of public consciousness, understanding the intricacies of treatment not only from a healthcare perspective but also from a business standpoint becomes crucial. This blog aims to demystify the complex relationship between treating substance abuse and mental health issues and the underlying business processes that make it possible.
Substance abuse and mental illness are not just personal struggles; they are also public health issues with significant economic implications. By examining the business process behind treatment, we better understand how resources are allocated, how services are priced and provided, and how the industry adapts to the ever-evolving mental health and addiction therapy challenges.
Join us as we embark on a comprehensive journey through the realms of healthcare and business in the context of substance abuse and mental illness treatment. Our exploration will provide insights for healthcare professionals, business leaders, policymakers, and anyone interested in the nuanced intersection of health and commerce.
Window of Opportunity
- The big book refers to a “window of opportunity” – a time when he or she is most “teachable.”
- “If he says ‘right now I want help’, and you don’t do it right at that moment, then he could change his mind in a matter of 20 minutes.”
- When someone struggling with addiction reaches out for help, it is critical the person helping responds immediately and finds help right away.
- Otherwise, one of three things will happen – the person suffering will go back to using, end up in jail, or end up dead.
Program Options
Private – generally accepts commercial insurance, needs to verify benefits before
admission, and competes against other centers admitting clients and verifying
benefits.
Nonprofit – sometimes accepts commercial insurance but usually doesn’t anticipate
the same level of revenue per client as private centers. It is not as competitive with the
private centers.
Government funded / free program – usually funded through grants, donations, or
program generated revenue. Typically, it doesn’t compete against private/nonprofit
Organizations.
| Category | Type | Description |
|---|---|---|
| Core Business | Detoxification Units | Provide detox services |
| Treatment Centers: Inpatient Only | Offers Residential/PHP Services | |
| Treatment Centers: Inpatient/Outpatient | Offers PHP/IOP/OP Services | |
| Treatment Centers: Outpatient Only | Offers IOP/OP Services | |
| Supportive Businesses | Laboratories | Provides confirmation drug testing |
| Billing Companies | Provides billing, utilization, and verification services | |
| Lead Generations | Provides clients to centers | |
| Software/Tech | Electronic Health records, lab interface software, billing software | |
| Ancillary Recruitment | Providers qualified human capital |
Organizational Structures
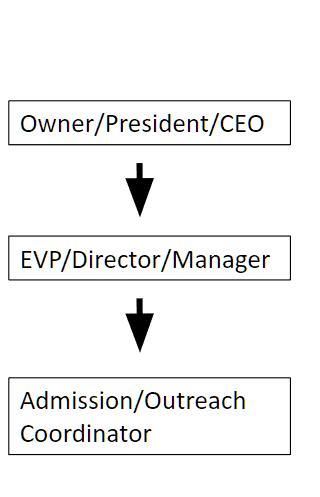
Most organizations have the same corporate structure on the business development/sales/marketing side. Usually, these are the roles:
Owner/President/CEO (decision maker)
EVP/Director/Manager (decision maker/influencer)
Admission/Outreach Coordinator (influencer)
These positions may be filled by one person or several, depending on the size of the organization.
Admissions Process
When someone needs help, they either find treatment options themselves or ask someone else for help. In fact, if you were to call a center the first thing they would ask you is if you are calling for yourself or someone else.
Someone else could be a family member, friend, co-worker, pastor, trust manager, attorney, boss, etc.
The admissions/outreach person (call center rep) at the center will determine qualification and will either accept the person needing help into treatment or refer the person needing help to another center.
| Qualifications | Examples |
|---|---|
| Financial | Insurance, Self-Pay, Scholarship |
| Clinical | Mental Health Needs, Heavy Psych, Schizophrenia, Suicidal Risk |
| Medical | Health Issues, Medications, Recent Surgeries |
| Physical | Mobility, Pregnancy |
| Legal | Upcoming Court Appearances, Allowed to leave the state |
| Age | Adolescence, adult |
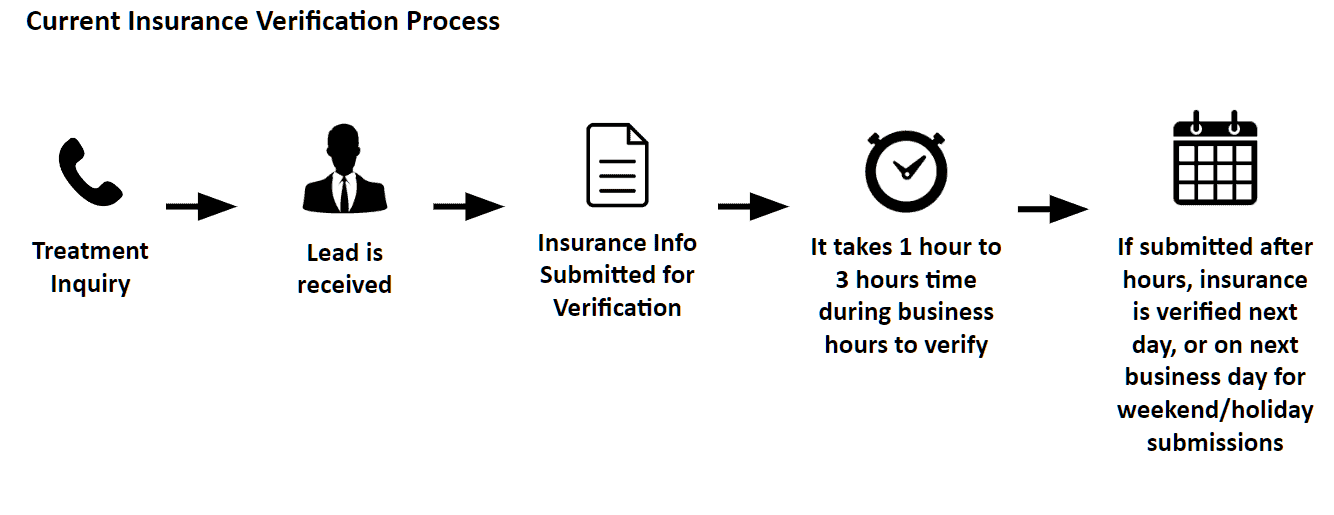
Unless clinical, medical, or physical issues are immediately identified, one of the first steps in the process is determining whether or not the insurance will reimburse for treatment and/or if the person has the financial ability to pay.
A verification of benefits (abbreviated “VOB”) is completed to determine insurance coverage (i.e., benefits and eligibility)
Once financial qualification is determined and approved (i.e., the insurance is accepted at the center), an initial screening is completed to identify clinical, medical, physical, and legal issues.
Initial screening is usually done over the phone and takes about 30 minutes to complete.
ASAM criteria are used to determine the level of care needed for treatment.
ASAM Criteria for Admissions
These factors determine the level of care needed to treat the patient:
Level of intoxication and/or withdrawal potential
Presence of other medical conditions
Presence of other emotional, behavioral, or cognitive conditions
Readiness or motivation to change
Risk of relapse or continued drug use
Recovery environment (e.g., family, peers, school, legal system)
Read more on ASAM Criteria.
| Level Of Care | Description |
|---|---|
| Detoxification (Detox)
Average Cost for Detox – $10,000 Typically, 3 days to 7 Days length of stay |
|
| Levels of Care | Description |
|---|---|
| Residential (RES)
Average Cost For Residential – $ 12,000 Typically, 7 Days to 30 Days Length of Stay |
|
| Partial Hospitalization (PHP)
Average Cost for Partial Hospitalization – $15,000 Typically, 14 days to 45 days length of stay |
|
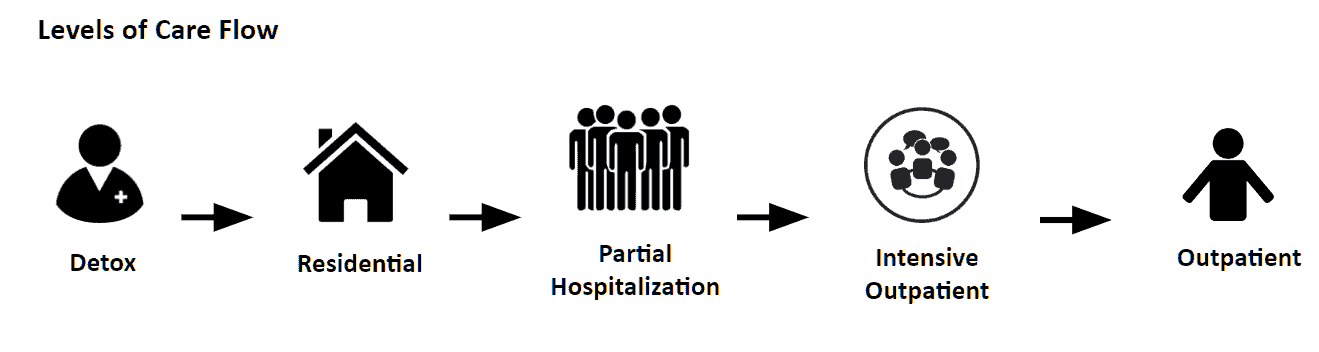
Treatment Types (levels of care)
Detoxification (Detox) – Provided on an inpatient or outpatient basis to assist patients with withdrawal from alcohol and/or drugs. Patients are given medications (protocol) to help with withdrawal symptoms (like shakes & sweats) and to avoid seizures. Length of stay – generally 72 hours to 120 hours of 24-hour medically surprised care to ensure safety or given medication to take on an outpatient basis. Insurance typically requires pre-authorization for services rendered based on medical necessity.
Residential (Res) – 24-hour per day, supervised care (step down from detox) typically in a non-hospital like setting. Patients (clients) generally stay in a therapeutic community and receive group and individual counseling. Length of stay – generally 1 week to 30 days. Insurance typically requires pre-authorization for services rendered based on medical necessity.
Partial Hospitalization (PHP) – a (step down from residential treatment) intensive outpatient psychiatric day treatment program that is furnished as an alternative to inpatient psychiatric hospitalization. Patients admitted to a PHP must be under the care of a physician who certifies and re-certifies the need for partial hospitalization and require a minimum of 25 hours per week of PHP therapeutic services. Providers generally continue to house their patients. Insurance typically requires pre-authorization for services rendered based on medical necessity.
Intensive Outpatient (IOP) – The typical IOP program offers group and individual services of 10–12 hours a week. IOP allows the individual to be able to participate in their daily affairs, such as work, and then participate in treatment at an appropriate facility in the morning or at the end of the day. Length of treatment is about 30 to 90 days. Some treatment providers continue to house patients, or make accommodations at sober homes (also called halfway house). Insurance typically requires pre-authorization based on medical necessity.
Outpatient (OP) – the least intensive form of treatment, generally 1 to 3 times a week for 45 minute to 1.5 hour individual or group sessions. Insurance typically does not require pre-authorization based on medical necessity.
After the person needing help meets all levels of qualification, intake is arranged and the person needing help is admitted into the appropriate level of care, based on medical necessity.
Information and Trends
As of 2024, the Substance Abuse and Mental Health Services Administration (SAMHSA) has proposed a significant increase in its budget to address mental health and substance use services across the United States. The proposed budget for SAMHSA in Fiscal Year 2024 is $10.8 billion, a substantial increase from the previous year’s budget. This funding is aimed at addressing various aspects of mental health and substance use disorders, including prevention, treatment, and crisis care.
The budget includes specific allocations for treating the opioid disorder epidemic and for providing substance use disorder (SUD) treatment and prevention services. A portion of this funding, approximately $5.7 billion, is dedicated explicitly to substance use prevention and treatment activities. This represents a $1.3 billion increase from the FY2023 budget.
The budget also proposes $4.9 billion for mental health activities, an increase of $2.2 billion from the previous year. These funds are intended to support community programs, pediatric behavioral health services, and assistance for individuals with serious mental illnesses.
In terms of the state of mental health in the United States, recent data shows that a significant percentage of adults and youth face mental health challenges and substance use disorders. However, many of these individuals do not receive the treatment they need. Key findings from Mental Health America indicate that in 2019-2020, about 20.78% of adults were experiencing mental illness, which is equivalent to over 50 million Americans. Additionally, 15.35% of adults had a substance use disorder in the past year, but 93.5% of them did not receive any form of treatment.
These statistics highlight the ongoing need for increased access to mental health and substance use disorder treatments and the importance of the proposed increases in funding and resources to address these challenges.
You can visit the SAMHSA website and Mental Health America’s report here for more detailed information.
Competition
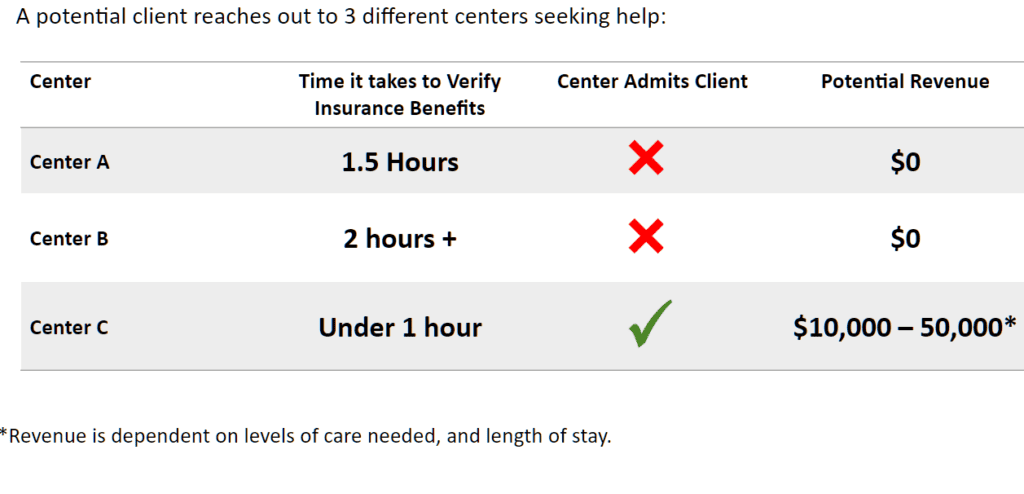
The world of substance abuse and mental health treatment isn’t just about offering crucial care; it’s also a field marked by intense competition. Imagine this: You’re searching online for help, typing in ‘alcohol treatment’ or ‘drug treatment’. You’ll find a sea of ads, each promising support and healing, a reflection of just how many are vying to reach those in need first.
In this crowded space, it’s not just about the care offered but also how quickly a treatment center responds. Someone reaching out for help might contact several places, but often, the first one that says ‘yes’ is where they end up going. This rush to respond first isn’t just about filling beds; it’s a sign of how these centers navigate the tightrope between health care and business. They’re in a race to offer help and ensure their business survival in a highly competitive market.
This situation paints a vivid picture of the current state of the substance abuse and mental health treatment industry. It’s a world where the urgency of healthcare needs meets the brisk pace of business, where every call for help is an opportunity for a center to demonstrate its commitment to care and a chance to stay afloat in a sea of competition.