"What used to take us over an hour now takes minutes. The intake team doesn’t need to rely on us anymore just to verify benefits."
%
See co-pays, deductibles, and behavioral health carve-outs in real time. Go beyond "active" status to make confident financial decisions. Know patient responsibility upfront—before admission, not after discharge.
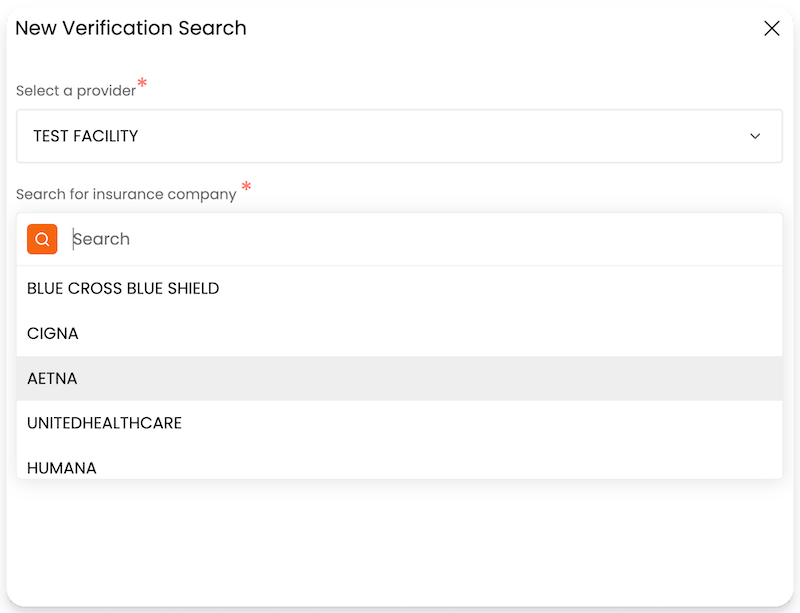
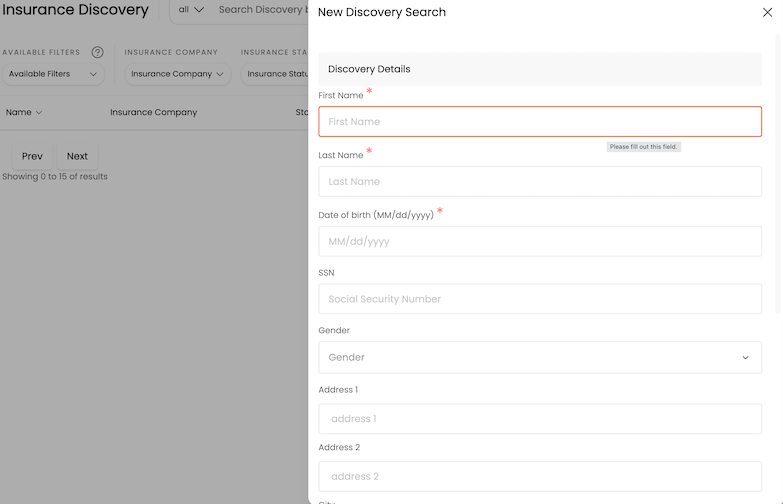
Locate active Medicaid coverage even with incomplete patient data. Reduce verification dead-ends and uncover billable policies. A unique capability most Medicaid verification tools lack.
Automatically flag inactive Medicaid policies across your entire census. Catch the root cause of 85% of eligibility denials before claims go out. Most facilities find at least one lapsed policy per week—that's $7-10K saved every time.

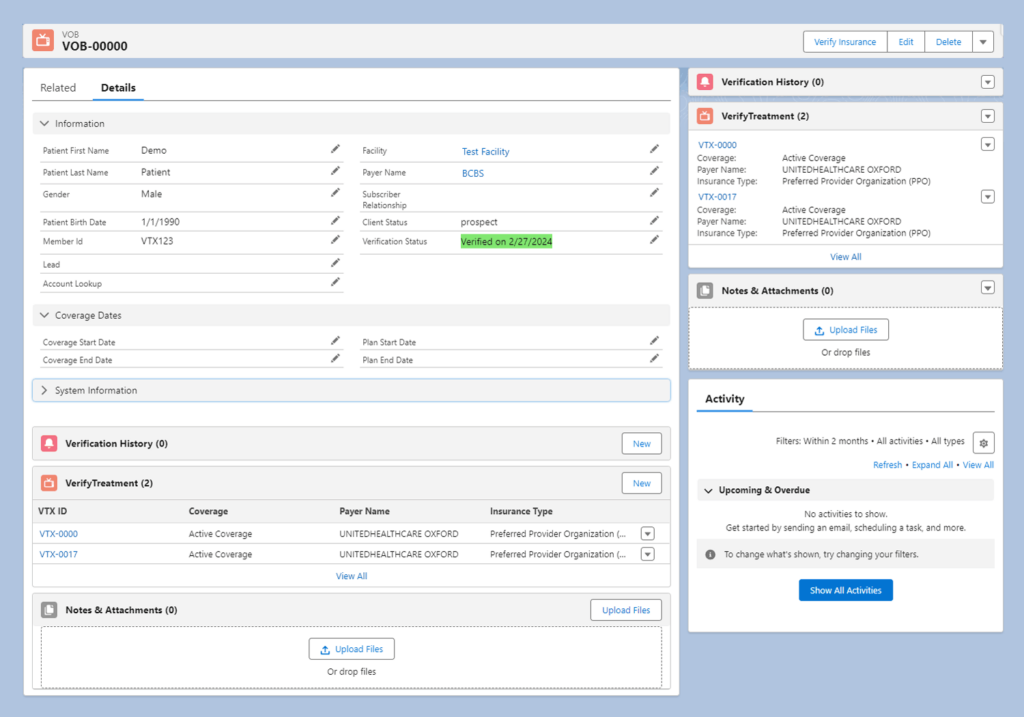
Run Medicaid verifications and attach results directly to contact records. Eliminate duplicate entry and ensure perfect admissions-to-billing handoffs. Keep your workflow in one system.
Automated alerts for benefit changes, authorization requirements, and Medicaid carve-outs, logged as internal payer notes so admissions has clarity before intake. Provide clear patient financial responsibility upfront.

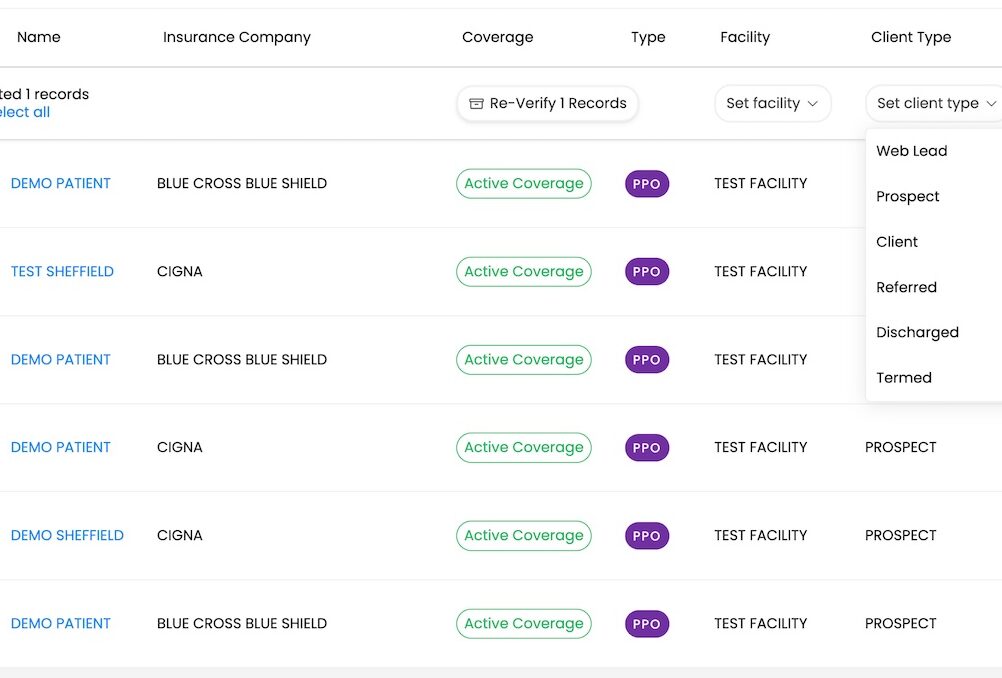
Manage Medicaid eligibility across all 50 states in one login. Our platform handles state-specific rules and system nuances, so expanding services or opening new locations doesn't break your verification workflow.

VerifyTX delivers near-immediate benefit verification at your agents’ fingertips.
Simple to install and configure, easy to extend with Salesforce, and backed by a responsive, collaborative team. We tried multiple solutions before switching and are glad we did. Painless, effective, and affordable.
You’ll see the full financial picture needed for behavioral health: coverage dates, member IDs, co-pays, deductibles, and—critically—detailed benefits for SUD and mental health treatment levels (e.g., inpatient residential, intensive outpatient). We show you the carve-outs and authorizations so you know exactly what is covered before admitting.
Up to 85% of denials stem from eligibility issues like inactive policies or missed coverage changes. Our platform provides real-time, accurate data and includes automated lapse detection that actively monitors your census for terminated coverage. This allows you to address problems before services are rendered and claims are submitted.
Yes. Unlike calling state Medicaid offices, our real-time system is available 24/7/365. This is essential for admissions teams handling intake calls during evenings, weekends, and holidays, ensuring you never miss an opportunity to help someone ready for treatment.
It works natively inside your CRM. Install the VerifyTX component, and your team can run a verification from any lead, contact, or account record with one click. All results—coverage details, notes, and the verification timestamp—are written back to the record. This eliminates duplicate data entry and creates a perfect handoffs.
Our insurance discovery feature locates active Medicaid and commercial policies even with incomplete data. This drastically reduces "no insurance found" dead-ends and helps you locate billable coverage that manual verification misses.
All 50 states. Our platform accesses 1,700+ payers, including state Medicaid programs, Medicaid managed care plans, and commercial insurers. We handle state-specific rules and system differences automatically.
Most clients are up and running in days, not months. Because our platform is cloud-based, not a legacy enterprise system, implementation is fast. Our team handles setup and provides dedicated support to ensure your team is successful.

Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.