“We had 85% of denials tied to eligibility. Fixing that started with knowing which payers need what — and VerifyTX gave us that visibility.”
%
Use a 1-to-5 star system to track payer reliability as you learn which plans approve quickly, reimburse consistently, or cause claim headaches. Star ratings appear instantly during every VOB, so your team knows what to expect before saying yes.

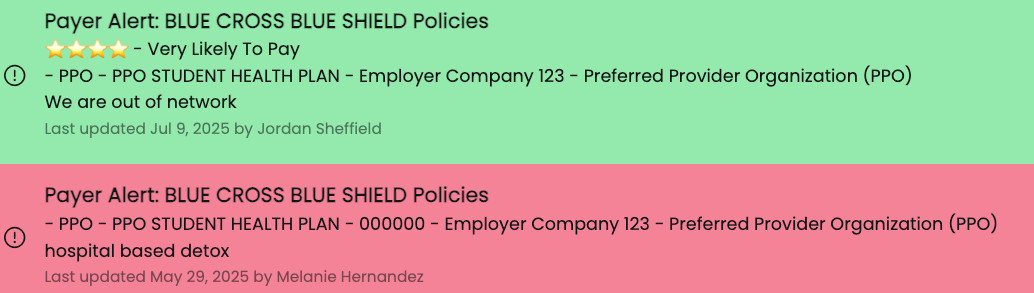
Add custom notes tied to specific payers, groups, or employers—pre-auth phone numbers, network restrictions, out-of-pocket collection requirements. Alerts appear automatically when those plans come through, so nothing gets missed in the moment.
Create alerts by insurance type, group name, or employer. Use color coding to flag risk levels and send optional email alerts for high-priority cases. It’s all flexible and built around how you operate.


New hires, weekend staff, and billing teams all see the same institutional knowledge. No more "let me ask someone who's been here longer" or expensive mistakes from teams working in the dark.
Payer Alerts are customizable notes that surface during eligibility checks to flag payer-specific quirks like prior auth requirements, claims addresses, or known denial patterns so your staff doesn’t miss critical steps.
Anyone with VerifyTreatment access can view alerts. Admins and RCM leads can create and update alerts across all users and batches
Yes. Alerts are visible in both manual and scheduled batch verifications. You can also tag specific clients to include them in automated runs
Common examples include
• Claims submission addresses
• State-specific Medicaid carve outs
• Union payer rules
• Prior auth fax or phone contacts
• Flags for SUD versus MH coverage separation
Alerts are fully client controlled. While import functionality is coming soon, many teams start by manually logging key payer quirks like Blue Cross MCO behavior or UHC mental health carve outs

Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.