

Thoughtful AI uses managed bots to handle back-end revenue cycle work such as eligibility checks, claims processing, and payment posting. Pricing is custom, but many organizations report costs starting around $7,500 upfront per bot and about $1,500 per month, with total spend increasing as more workflows are automated.
If your billing team is spending hours on eligibility follow-ups, claim fixes, or payment posting, automation can start to look less like a nice-to-have and more like a necessity. Thoughtful AI is built for that reality, using managed bots to handle routine revenue-cycle work so your team can focus on exceptions.
That kind of support can be valuable, but the cost still needs to fit your workflow and volume. Thoughtful AI is sold as a managed service, with custom pricing that usually includes an upfront setup fee and a monthly cost per bot, with total spend increasing as you scale.
Below, we break down what Thoughtful AI typically costs, what you get for that investment, and where the model tends to fit best.
Our perspective comes from supporting real-world revenue and admissions workflows, not just evaluating automation features.
Today, 4,000+ programs rely on our platform and its connections to 1,700+ payers, so we see firsthand how pricing, workflow fit, and operational impact play out over time.
You can book a free demo today.
Unfortunately, thoughtful AI does not publish standard pricing. Each deployment is quoted through a sales process based on the work you want to automate and how much volume you handle.
Most projects include two main costs, though:
Your final price depends on a few factors:
For larger deployments, pricing is often bundled and negotiated instead of charged per bot. Contracts are usually tied to expected results, such as time saved or reduced manual work.
This model can make sense for billing-heavy teams. But as you add more workflows or volume, costs tend to grow, so it’s important to evaluate scope early.
Related: See what the reviews say about Thoughtful AI.
So, what does paying for Thoughtful AI actually buy you? In broad terms, you’re paying for automation delivered as a service.
Thoughtful’s team will design and maintain software bots that log into systems and perform tasks just like a human would, only faster and error-free. At the price point we discussed, you can expect the following core capabilities and benefits:
Thoughtful AI focuses on billing and revenue-cycle tasks that take up a lot of staff time. Bots can handle eligibility checks, claim submission, payment posting, and some denial workflows. These tasks run in the background, with human review available when something falls outside the rules. For billing teams, this can reduce repetitive work and help keep queues moving.
You don’t need an internal RPA or automation team. Thoughtful designs the workflows, keeps bots running, and updates them when payer portals or rules change. That removes IT overhead, but it also means you’re relying on an external team to adjust or expand automation over time.
The platform is tuned for measurable RCM results like fewer denials or faster payment posting. Many customers evaluate Thoughtful based on time saved or improvements in collections. That makes it a good fit for billing-heavy operations, where small efficiency gains can add up.
These strengths make Thoughtful AI a strong option for revenue cycle teams. If your challenge is high claim volume, limited billing staff, or too much manual rework, this kind of automation can help keep back-office work moving.
However, for intake-driven organizations (like behavioral health admissions teams), Thoughtful AI can fall short in important ways.
The platform’s DNA is in RCM, basically optimizing the billing cycle after a patient is seen. It’s not originally designed as an admissions-front-end tool, and that shows in a few limitations.
Here are a few limitations to be aware of:
Admissions teams often need answers while a patient or referral source is on the phone. Thoughtful can run eligibility checks, but results may come through background workflows rather than an instant, user-driven search.
When decisions depend on immediate clarity, that delay can slow the conversation or push follow-up to later.
Behavioral health intake usually depends on more than active or inactive status. Teams often need to understand level-of-care limits, authorization needs, or behavioral health carve-outs. A general RCM workflow may confirm coverage, but staff may still need to dig deeper to understand what treatment is actually covered.
Thoughtful integrations are strongest on the billing side. Admissions teams using Salesforce or other intake systems may not see verification details directly in their workflow, which can lead to extra steps or handoffs between departments.
Thoughtful’s value is easier to measure in billing efficiency or denial reduction. For admissions, the impact often shows up as faster decisions or fewer lost inquiries, which can be harder to tie directly to a cost model.
All in all, Thoughtful AI works well for the work it was designed to handle. But for organizations where verification needs to support real-time intake decisions, it may feel more like a back-office tool than a front-end solution.
It can be made to help with intake to some extent, but it won’t feel like a perfectly tailored solution for admissions staff. This realization has led many behavioral health providers to seek a different approach for their insurance verification needs – one geared from the ground up for intake operations.

For teams where insurance verification drives admissions decisions, the priority is speed and clarity at the front end. That’s where our platform is different. VerifyTreatment was built specifically for behavioral health admissions, not adapted from a general medical billing workflow.
Instead of treating eligibility as a back-office task, we focus on the moment it matters most, when your team is deciding whether and how a patient can move forward.
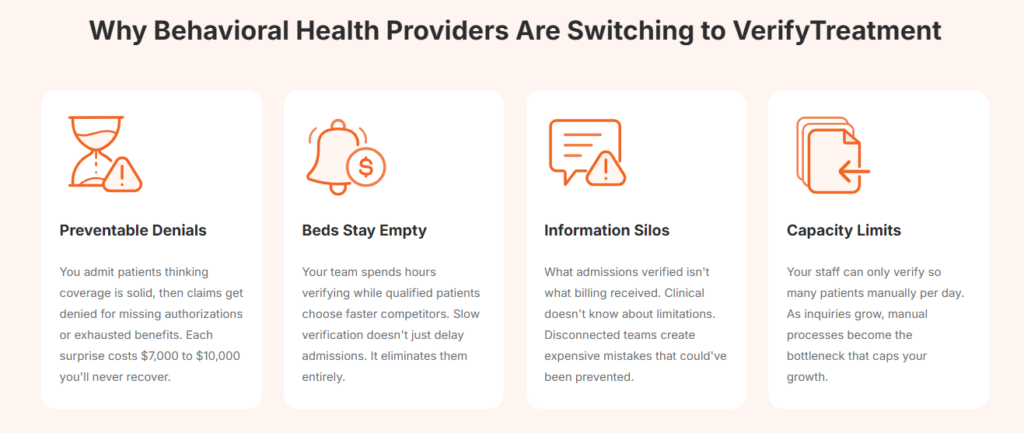
Behavioral health coverage is rarely simple. Carve-outs, level-of-care limits, authorization rules, and state-specific plan differences all affect the decision.
VerifyTreatment surfaces coverage in a way that aligns with treatment questions, not billing codes. Your team can see what applies to detox, residential, PHP, or outpatient care, along with key financial details, without having to interpret raw payer responses.
Admissions conversations move quickly, and waiting on background processes can slow things down.
VerifyTreatment is designed to return detailed benefit information in seconds so your team can review coverage while the caller is still on the phone. Mobile and browser access support after-hours and on-the-go use without adding extra steps.
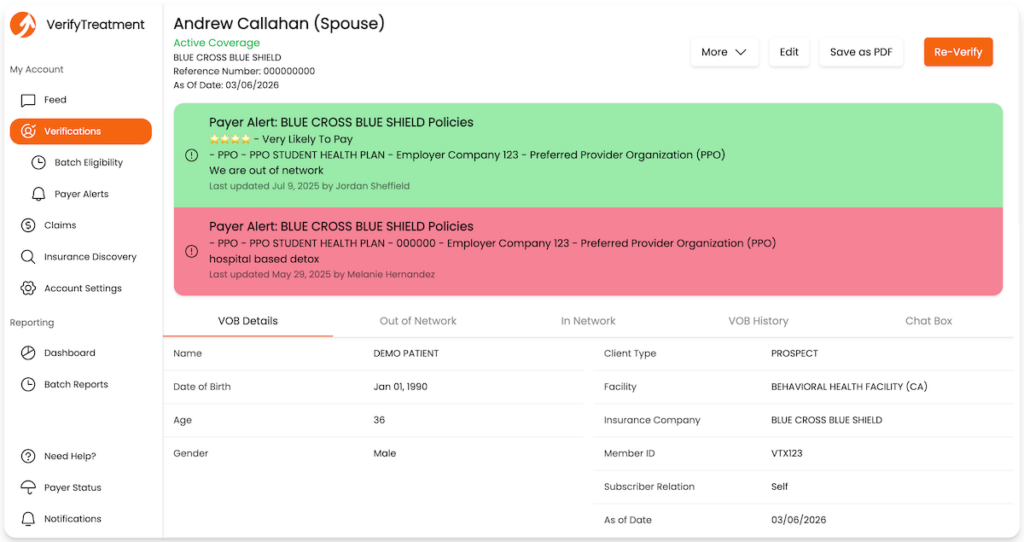
Basic eligibility checks often confirm only that a policy exists. Intake decisions usually require more context.
VerifyTreatment provides:
This helps reduce follow-up calls and limits surprises that tend to surface later in billing.

Many inquiries start with limited or outdated details. Patients may not have a card, may be unsure of their plan, or may have recently changed coverage.
VerifyTreatment can locate active policies using partial information, helping teams avoid self-pay assumptions and recover admissions that might otherwise be lost.
Coverage issues do not always show up at intake. Plans change, policies lapse, and managed care rules shift during treatment.
VerifyTreatment supports:
This helps teams address issues earlier instead of finding them after revenue is at risk.
Admissions and billing often work from different information, which leads to rework and confusion.
Verification results stay connected to the patient record and can integrate with systems like Salesforce. Everyone works from the same data, which supports cleaner handoffs and fewer follow-up questions.
Because the platform is purpose-built, implementation is typically lighter than a custom automation project. Teams can get started quickly, and verification workflows continue to hold up as census grows, new locations open, or payer mix changes.

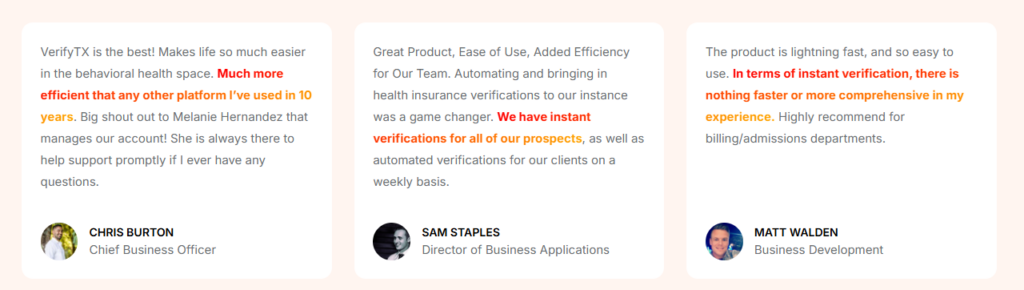
That said, organizations often turn to VerifyTreatment after delays or uncertainty begin affecting admissions. Foundations Recovery Network, for instance, reported losing roughly 1 in 10 admissions due to slow insurance answers.
After moving to VerifyTreatment, they reduced those delays, recovered more than $10,000 per month in previously lost revenue, and were able to give families clearer financial information earlier in the process.
If insurance questions are slowing intake, earlier visibility can help. VerifyTreatment gives your team real-time benefit details during admissions, so decisions don’t have to wait and coverage issues are easier to catch early.
The quickest way to evaluate the fit is to see it in action. In a short demo, you can watch a live verification, review the benefit detail that appears, and see how the workflow supports admissions and billing.
Book a demo to see how VerifyTreatment works in real intake scenarios.
Disclaimer: All trademarks, logos, and brand names are the property of their respective owners. The use of any third-party trademarks, logos, or brand names in this article is for informational and comparative purposes only, and constitutes nominative fair use. This article was published by VerifyTreatment, and while we strive for objective comparisons, VerifyTreatment is included as an option within this list.




Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.