
VerifyTreatment is the strongest Waystar alternative for behavioral health providers. It’s purpose-built for intake-first verification, deep payer logic, and admissions-to-billing clarity. For an all-in-one EHR and billing system, Kipu Health and Qualifacts are worth considering.
Waystar is a powerful enterprise RCM platform built for high-volume billing and large provider networks. It makes sense if you’re running a hospital chain.
But behavioral health (BH) providers and SUD treatment programs operate differently. Admissions decisions depend on real-time eligibility, payer carve-outs, and managed care nuances most enterprise tools weren’t designed for. A missed detail on a Medicaid or Medicare Advantage plan can mean a lost admission, or a denied claim weeks later.
This article covers 11 solid alternatives, but first, here are our top three picks:
| Pick | Best For |
| VerifyTreatment | Treatment centers, SUD programs, multi-state BH networks needing deep payer logic and intake-first verification |
| Kipu Health | BH treatment centers wanting an all-in-one clinical and billing system on a single EMR platform |
| Qualifacts | Large behavioral health agencies needing a full EHR and RCM system |
VerifyTreatment is a real-time insurance eligibility and RCM automation platform built specifically for behavioral health providers — by people who understand admissions and billing in treatment settings.

VerifyTX is the best! Makes life so much easier in the behavioral health space. Much more efficient than any other platform I’ve used in 10 years. Big shout out to Melanie Hernandez that manages our account! She is always there to help support promptly if I ever have any questions.
We regularly speak with treatment centers evaluating or replacing platforms like Waystar, which means we know exactly where enterprise tools create gaps in behavioral health admissions and billing.

Waystar is a cloud-based RCM platform combining clearinghouse services, claims management, eligibility verification, payment processing, and AI-driven analytics.
Its strength is breadth — Waystar handles enterprise-level revenue cycle operations across diverse provider types at scale.
In hospitals, revenue cycle workflows are largely claims-driven and happen after the encounter. Whereas, in behavioral health and SUD treatment programs, financial payer carve-outs directly determine whether a patient can be admitted.
That makes eligibility depth far more critical in behavioral health than in many other provider settings.
Admissions coordinators are often verifying insurance live on intake calls — sometimes after hours — while a patient or family waits for clarity. If eligibility requires multiple portal checks or follow-up calls, it creates coverage surprises that delay admissions or kill them entirely.
Many enterprise tools stop at confirming whether a policy is active. BH providers need to go deeper as admissions typically depend on understanding:
An active policy doesn’t guarantee reimbursable treatment. Deeper payer logic helps you avoid patient admissions under plans that won’t reimburse at the expected level, and finding that afterward is expensive.
Admissions teams don’t always receive complete policy information on the first call. When coverage can’t be located quickly, staff resort to manual follow-ups and callbacks, or chase insurance cards after a patient is already admitted. The ability to locate coverage from partial patient data isn’t a nice-to-have — it’s a daily operational need.
In behavioral health, reimbursement is highly sensitive to plan details, authorization requirements, and policy lapses. When eligibility depth is insufficient at intake, the impact surfaces later as denied claims, underpayments, or retroactive coverage issues.
For many providers switching tools, reducing eligibility-driven revenue leakage before admission is the primary goal.
Before going into a more detailed breakdown, here’s a snapshot to help you find the tool that fits how your team actually works.
| Platform | Category/ Strength | Key Features | Pricing | Best For |
| VerifyTreatment | Behavioral Health Eligibility and RCM | Real-time VOB, deep payer logic for behavioral health, insurance discovery with partial data, lapse detection, claim status, ERA, batch verification, Salesforce integration, API access and workflow embedding | Flexible and scalable with no user caps + 30-day money-back guarantee (entry-level plans often under $299 per month) | Behavioral health treatment centers needing deep payer logic, intake-first verification, and admissions-to-billing workflow clarity |
| Waystar | Enterprise RCM and Clearinghouse | Claims management, eligibility automation, intelligent edits, payer connectivity | Enterprise quote-based | Large health systems and hospital networks managing broad RCM operations |
| pVerify | Modular Eligibility Platform | Real-time eligibility, batch/API verification, insurance discovery, MBI lookup, claim status | Usage-based modular tiers | Multi-state or multi-specialty providers needing flexible, API-driven verification |
| Availity | Clearinghouse and Eligibility | All-payer clearinghouse, eligibility verification, claim submission, prior authorization | Free base tier; Pro pricing on request | Cost-sensitive practices needing broad payer access and basic eligibility functionality |
| Thoughtful AI | AI RCM Automation | Claims submission automation, prior auth management, payment posting, denial management | Quote-based | Billing teams looking to automate repetitive back-end RCM workflows |
| TriZetto | Clearinghouse and Claim | EDI connectivity, eligibility verification, ERA processing, claim status, denial management | Quote-based | Practices prioritizing clearinghouse infrastructure and claims submission workflows |
| Kipu Health | Behavioral Health EMR + Verification | EMR, clinical documentation, built-in eligibility verification, billing, claims management | Quote-based | BH treatment centers wanting an all-in-one clinical and billing system on a single EMR platform |
| Approved Admissions | Verification for Adjacent Markets | Eligibility verification, admissions workflow support, coverage discovery, claim status | Quote-based | DME suppliers, skilled nursing facilities, and billing companies needing admissions-focused verification |
| InstantVOB | Lightweight VOB Tool | Real-time eligibility, VOB reporting, multi-payer connectivity | Per-VOB and subscription tiers | Smaller practices needing simple, low-cost eligibility checks without full RCM complexity |
| athenaOne | Cloud EHR and RCM | EHR, eligibility verification, medical billing, claims management, patient engagement | Percentage of collections | Physician practices and medical groups consolidating clinical and billing operations |
| Qualifacts | Behavioral Health EHR and RCM | BH-specific EHR, integrated billing, eligibility verification, claims management, compliance reporting | Custom quote | Large behavioral health agencies and community mental health centers needing a full EHR and RCM system |
| Change Healthcare (Optum) | Enterprise Clearinghouse and RCM | Eligibility verification, claims submission, coverage discovery, payment processing, prior authorization | Enterprise quote-based | Large health systems and enterprise provider networks with high-volume RCM needs |
VerifyTreatment is a real-time insurance eligibility and revenue cycle automation platform purpose-built for mental health facilities, substance use disorder (SUD) treatment centers, and BH providers.
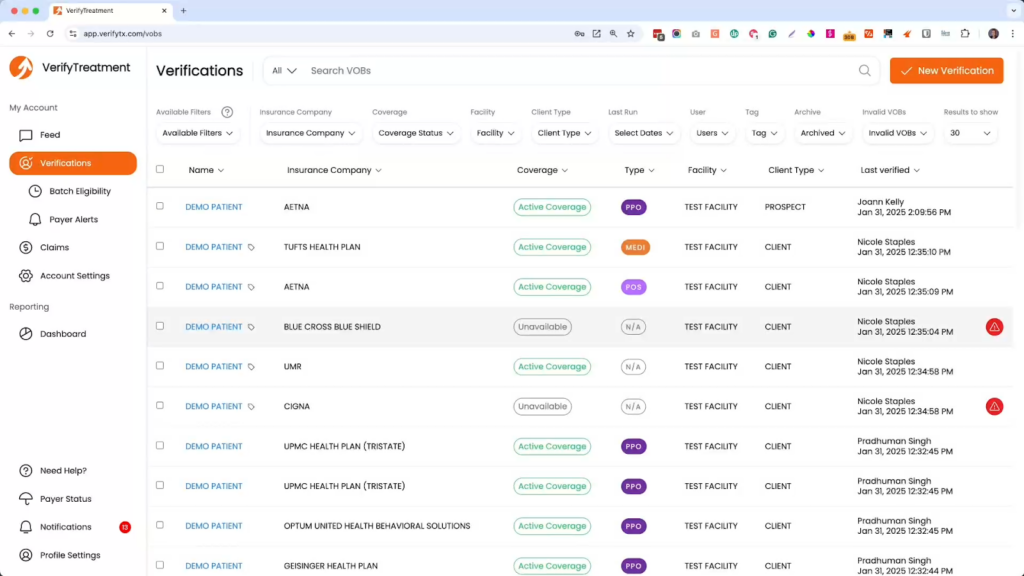
Unlike enterprise RCM platforms designed for hospital-scale billing operations, VerifyTreatment centers its architecture around admissions workflows, payer nuance, and preventing eligibility-driven revenue loss before a patient is admitted.
It’s the strongest fit for BH providers that need real-time, admissions-focused eligibility verification with deep payer logic and insurance discovery, especially for facilities verifying Medicaid, Medicare Advantage, and managed care plans at intake.
VerifyTreatment uses a tiered pricing model based on verification volume, feature activation, and operational scale. No user limits and you also get a 30-day money-back guarantee on all plans.
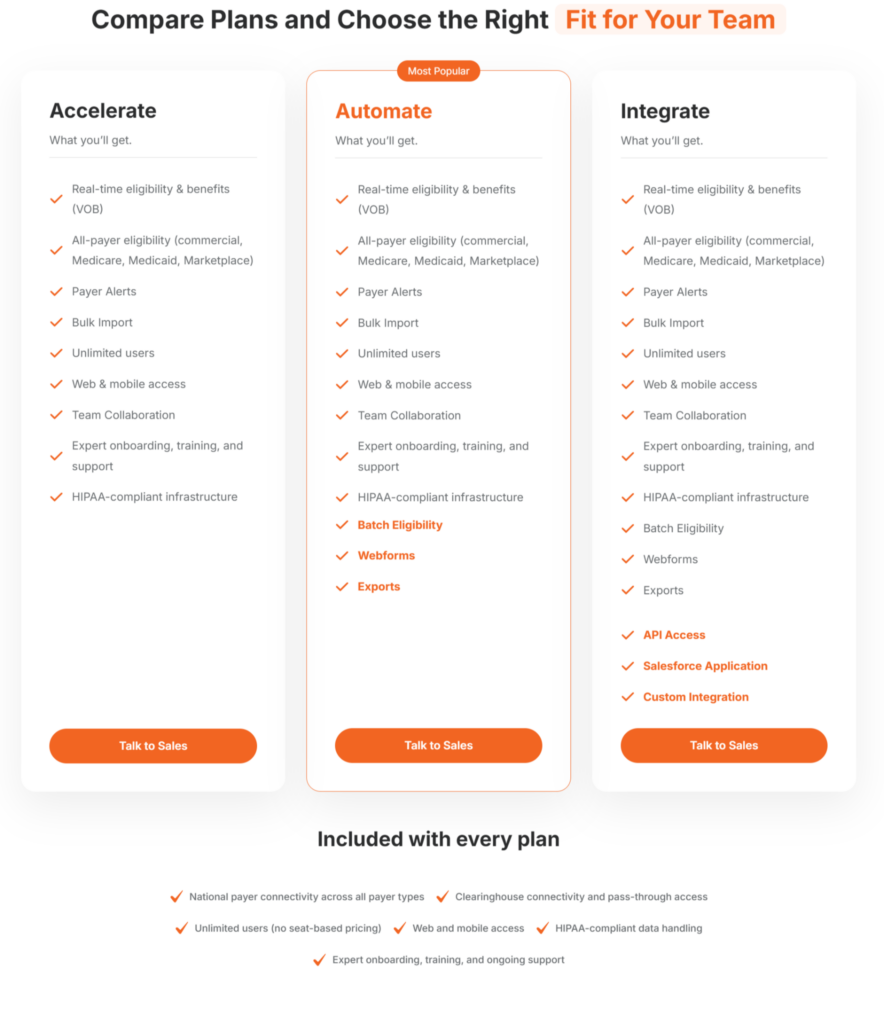
Entry-level plans are often under $500 /month, suited for single-location facilities with moderate verification volume.
Multi-location operators or high-census treatment networks may require expanded automation or API access.

I demoed other platforms, and they were all medical-focused with limited behavioral health benefits. VerifyTreatment was the only one built specifically for inpatient psych and residential behavioral health. That’s what stood out—it was tailored to us.

pVerify is an eligibility and verification platform built for a broad range of healthcare providers, including multi-state clinics.
It handles real-time eligibility, batch verification, and claims-related workflows through a flexible API-first architecture, connecting to 1,500+ payers
For BH providers, it can cover some verification needs, but its design reflects a general healthcare audience rather than the specific payer logic and carve-out depth SUD and mental health facilities typically require at intake.
pVerify uses a tiered subscription pricing model based on usage volume, solution type, and transaction limits.

Plans include Standard and Enterprise tiers across modules:
Availity connects providers with hundreds of payers through a centralized clearinghouse platform.
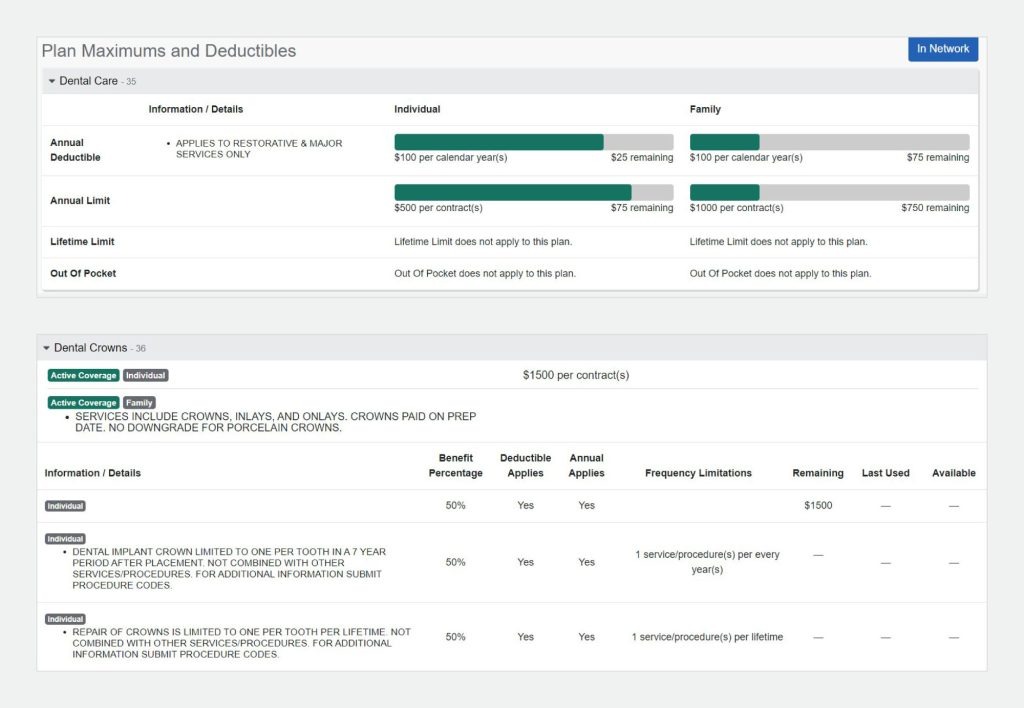
It offers broad payer access and solid infrastructure, but is built for general provider workflows rather than BH-specific intake processes.
Tiered structure with a free Essentials plan for basic payer access. Essential Plus at $25/month; Enterprise tiers from $28–$540/month.
Thoughtful AI is a revenue cycle automation platform that deploys AI agents to handle repetitive RCM tasks — working across existing EHRs, practice management systems, and tech stacks.

It’s not a standalone eligibility tool. But it excels in broad back-end RCM automation. Best for programs seeking to reduce manual workflows and operating costs without adding headcount.
Quote-based. No public pricing is listed.
TriZetto is a clearinghouse and RCM platform with deep EDI connectivity and a broad payer network.
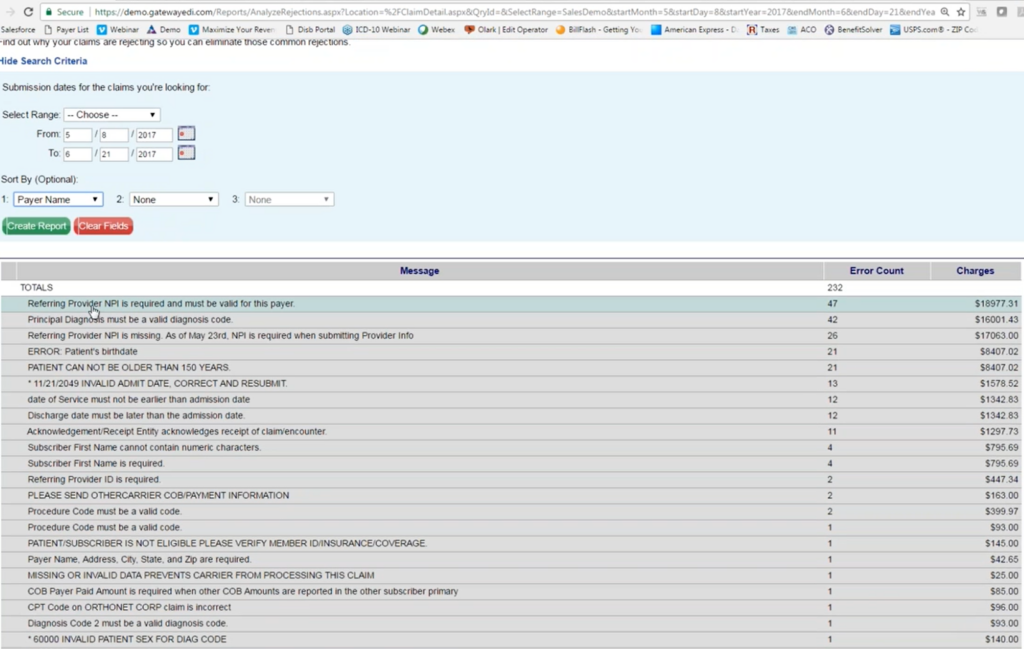
For BH providers, TriZetto’s strength is its clearinghouse infrastructure and claims workflows. This makes it a solid choice for practices that prioritize claims submission and remittance over front-end intake verification.
Quote-based. No public pricing is listed.
Kipu Health is a cloud-based EHR platform for clinical documentation, patient management, scheduling, and operational oversight within a centralized system. In addition to clinical functionality, Kipu includes billing and revenue cycle tools as part of its broader EHR workflow.
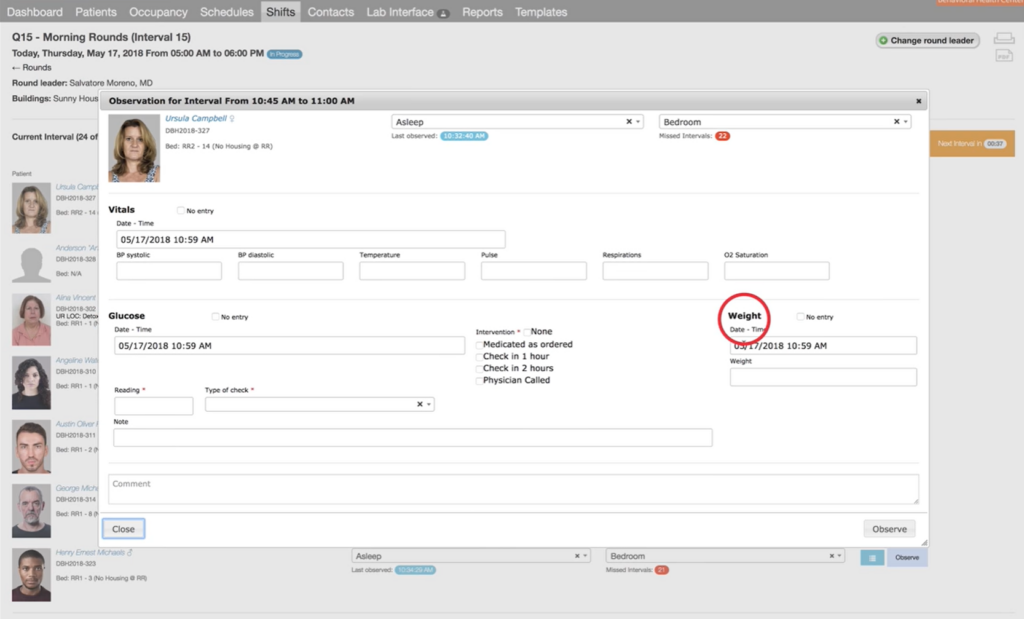
For providers already using Kipu as their clinical system, the built-in verification reduces the need for a separate tool. But it operates as a complement to the EMR, not a dedicated, depth-first eligibility platform.
Quote-based. No public pricing is listed.
Approved Admissions provides insurance eligibility verification and prior authorization services for a range of healthcare providers, including equipment suppliers, skilled nursing facilities, and billing companies.
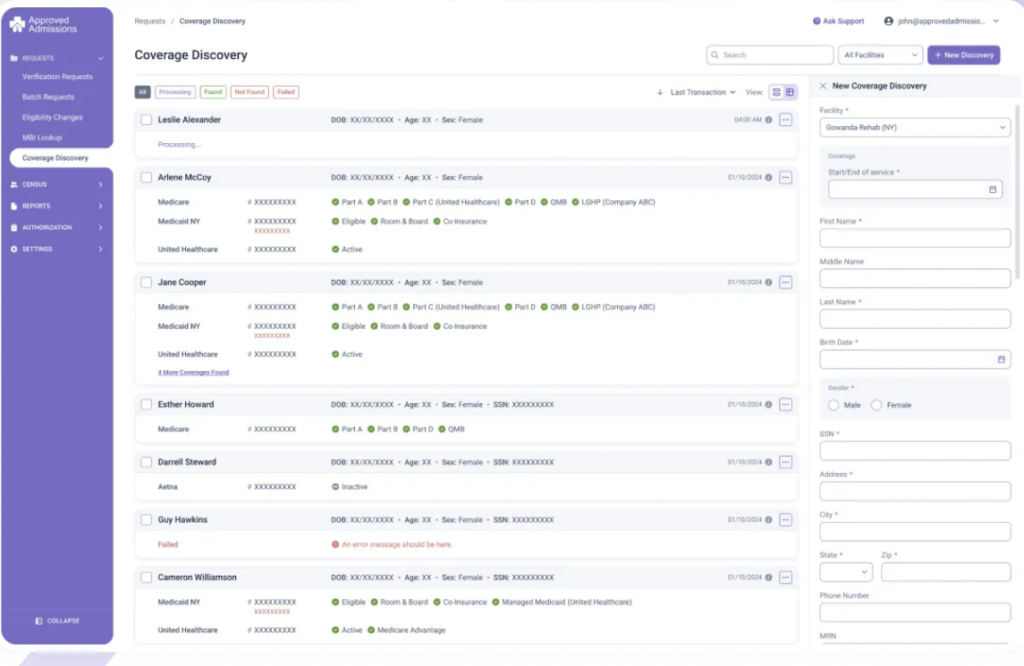
Because it serves varied provider types, its workflows aren’t built specifically around BH admissions.
Quote-based. No public pricing listed.
InstantVOB is a lightweight insurance verification tool for small-to-mid-sized clinics that need quick access to benefits information at the point of intake
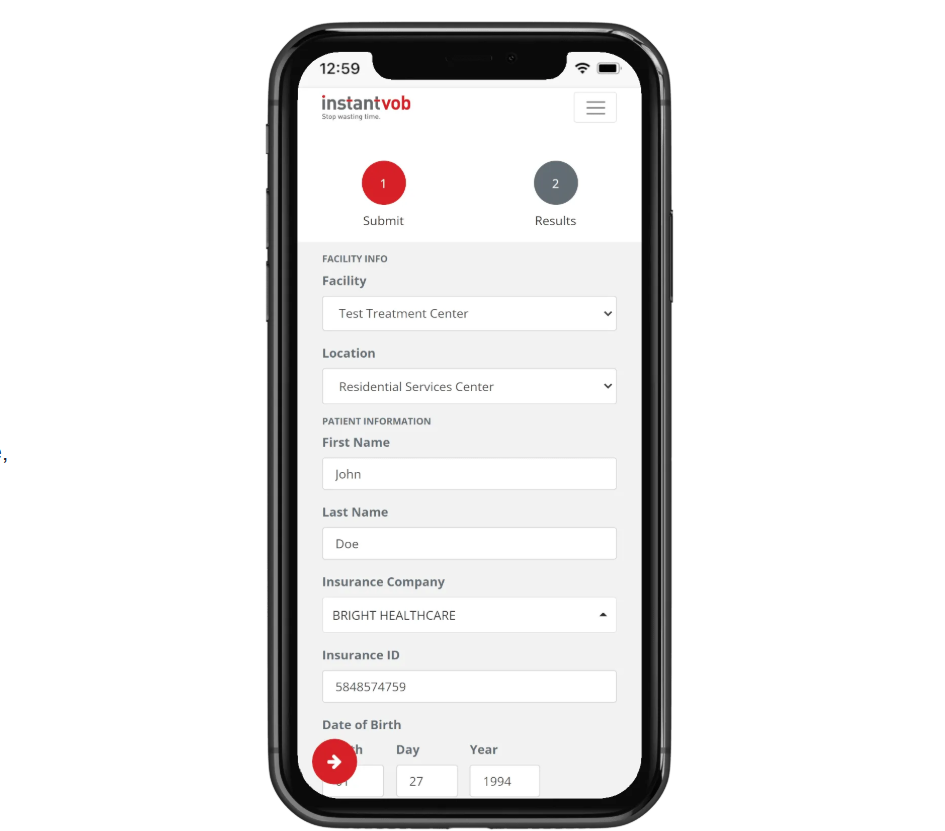
Its capabilities may not extend far enough for BH providers managing growing census, multi-state operations, or Medicaid-heavy payer mixes
InstantVOB uses a subscription model starting at $149.99/month, which includes up to 50 VOB queries. Plans scale with usage for small-to-mid clinics.
athenaOne combines EHR, practice management, patient engagement, and RCM into a unified system for ambulatory care providers. Its eligibility capabilities are designed for general medical workflows, not BH-specific admissions processes.
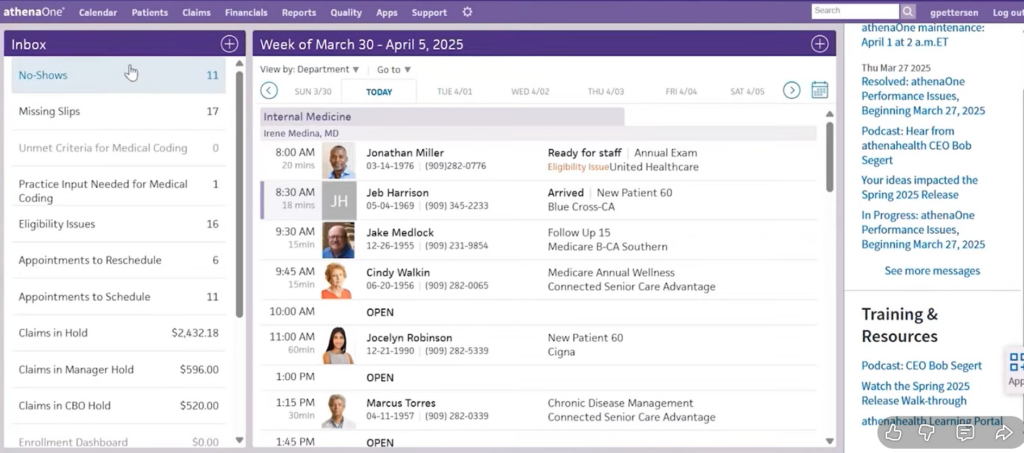
Quote-based, typically structured as a percentage of collections. No fixed public pricing.
Qualifacts is an EHR platform that provides clinical documentation, care coordination, and practice management tools for healthcare organizations.
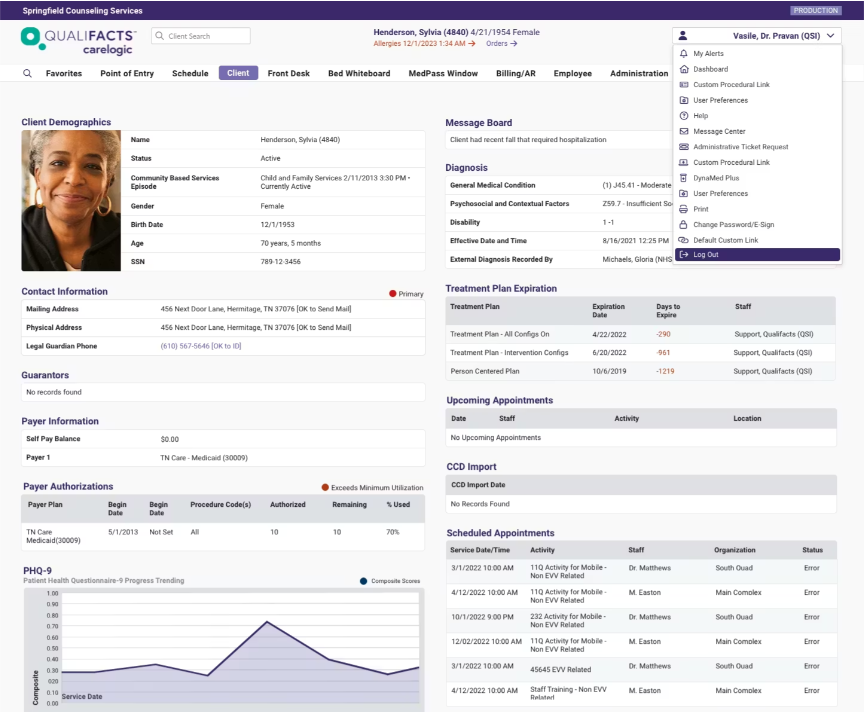
Qualifacts offers a portfolio of distinct electronic health record (EHR) products. Following a series of mergers and acquisitions, the company now maintains three primary, independent platforms tailored to different segments of the market: CareLogic, Credible, and Qualifacts InSync.
While the company has a strong presence in the behavioral health and human services space, its core focus remains EHR infrastructure. Eligibility verification and billing tools function as components of the EHR and revenue cycle modules.
Custom quote-based. No public pricing is listed.
Change Healthcare, operating under Optum, provides clearinghouse, claims management, payment processing, and eligibility solutions across the healthcare ecosystem. It’s built for large-scale connectivity, transaction processing, and interoperability across thousands of payers.

While it offers eligibility solutions at enterprise scale, its recent operational history are relevant considerations for any provider evaluating it as a Waystar alternative.
Enterprise quote-based. No public pricing listed.
Ultimately, choosing a Waystar alternative comes down to operational fit.
If you need an integrated clinical and billing system on a single EMR platform, Kipu Health or Qualifacts are worth exploring.
But if your treatment center is dealing with eligibility-driven denials, incomplete patient data, heavy Medicaid census, or admissions teams that can’t verify benefits on the first call, a broad RCM platform may not solve those problems. A behavioral health-specific one will. VerifyTreatment is built for exactly that.
If you’d like to see how it works in your admissions workflow, you can book a demo. All plans include a 30-day money-back guarantee.
Waystar is built for large health systems and broad provider networks. Treatment centers with intake-driven verification needs, heavy Medicaid census, or carve-outs may find it lacks the specialized payer logic their workflows require.
For intake-first eligibility verification built around behavioral health workflows, VerifyTreatment is the strongest fit. For an all-in-one clinical and billing system, Kipu Health and Qualifacts are worth considering.
It confirms active coverage and — at a deeper level — deductible status, out-of-network benefits, carve-outs, co-pay details, and payer-specific nuances critical for behavioral health admissions decisions.
Stop forcing your admissions team to use a general medical clearinghouse. Get the deep payer logic, carve-out alerts, and intake-first speed your facility actually needs.
Flexible plans with no user caps. Start your 30-day money-back trial today.Disclaimer: All trademarks, logos, and brand names are the property of their respective owners. The use of any third-party trademarks, logos, or brand names in this article is for informational and comparative purposes only, and constitutes nominative fair use. This article was published by VerifyTreatment, and while we strive for objective comparisons, VerifyTreatment is included as an option within this list.




Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.