

pVerify is a capable API-driven eligibility platform, reliable for general healthcare, weak on behavioral health depth. It has no lapse detection, no BH-specific payer logic, and no admissions-to-billing handoff. For treatment centers scaling intake or fighting eligibility-driven denials, VerifyTX is the purpose-built alternative.
pVerify does what it says: real-time eligibility checks, a broad payer network, flexible API architecture. For general healthcare verification, it’s a solid platform with a well-earned reputation.
However, for behavioral health, the question isn’t whether pVerify is good. It’s whether it’s the right fit. Carve-outs, SUD authorization requirements, Medicaid managed care nuances, and admissions-to-billing handoffs aren’t edge cases in behavioral health. .
They’re the core of how reimbursement works. A platform built for breadth across healthcare specialties handles them differently than one built specifically for this vertical.
This review breaks down what pVerify does well, the fit gets complicated for treatment centers, and why VerifyTX has become a leading alternative for behavioral health providers who need more depth.
Many eligibility verification reviews are written by people who understand billing software. This one is written by people who understand behavioral health billing.

VerifyTX is the best! Makes life so much easier in the behavioral health space. Much more efficient than any other platform I’ve used in 10 years. Big shout out to Melanie Hernandez that manages our account! She is always there to help support promptly if I ever have any questions.
VerifyTreatment works daily with admissions directors, billing and RCM leaders, and multi-state operators navigating the full complexity of behavioral health reimbursement — carve-outs, Medicare Advantage shifts, Medicaid managed care, and everything in between.
That’s the lens this review is written through — not a feature checklist, but the operational realities that determine whether a verification platform actually fits behavioral health.
pVerify is an API-driven SaaS platform for real-time insurance eligibility and benefits verification. It connects healthcare providers to a broad payer network and returns coverage data electronically.
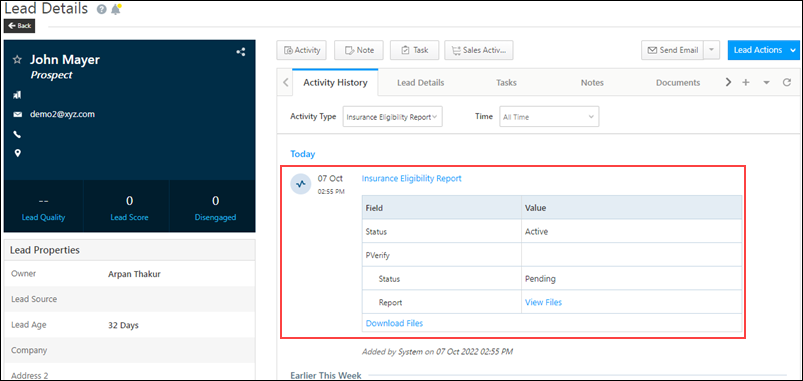
The platform supports multiple provider specialties, including primary care practices, hospitals, revenue cycle teams, and multi-specialty clinics. It’s designed to serve diverse healthcare environments rather than go deep on any single vertical. That breadth is strength in the right context. But for behavioral and mental health admissions teams, it can be a real limitation.
pVerify uses a modular, transactional pricing model with tiered plans and optional add-ons. However, there are no standardized or fixed public tiers. Organizations receive custom quotes based on selected modules, transaction volume, and integration requirements.
Here’s what the standard starting prices look like:
| Module | Standard Starting Price(Transactions/Month) | Enterprise Starting Price(Transactions/Month) |
| Advanced Eligibility | $125 (500) | Higher volume/custom |
| Insurance Discovery | $120 (80) | Higher volume/custom |
| MBI Lookup | $50 (75) | Higher volume/custom |
| Same or Similar | $190 (250) | Higher volume/custom |
| Certificate of Medical Necessity (CMN) | $100 (125) | Higher volume/custom |
| Claim Status | $40 (150) | Higher volume/custom |
| Skilled Nursing | $120 (150) | Higher volume/custom |
Because pVerify does not have fixed pricing tiers for behavioral health specifically, smaller and mid-sized treatment facilities may find it difficult to forecast total subscription costs without engaging directly with sales.
User reviews occasionally reference pricing surprises tied to additional modules or expanded usage.
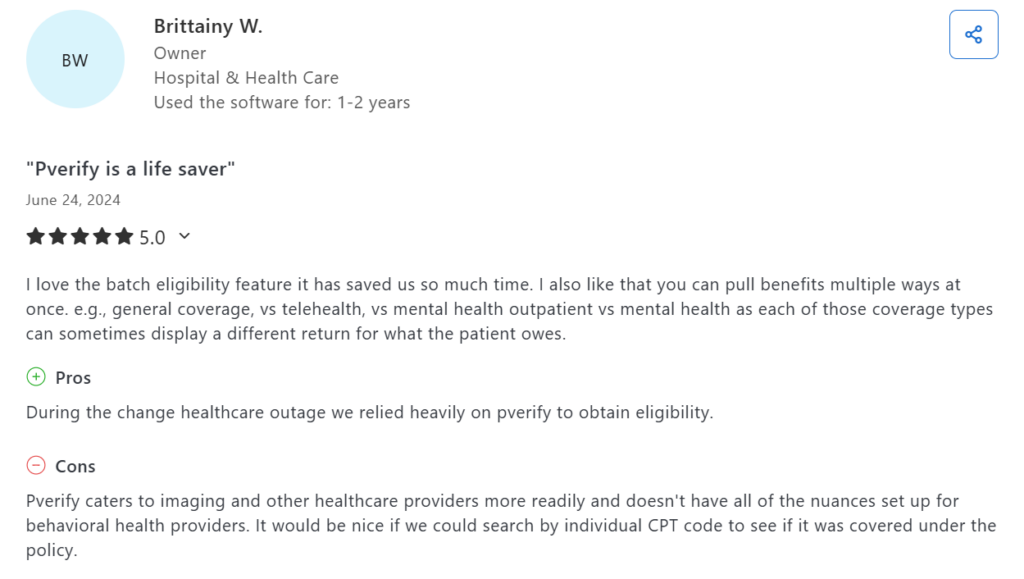
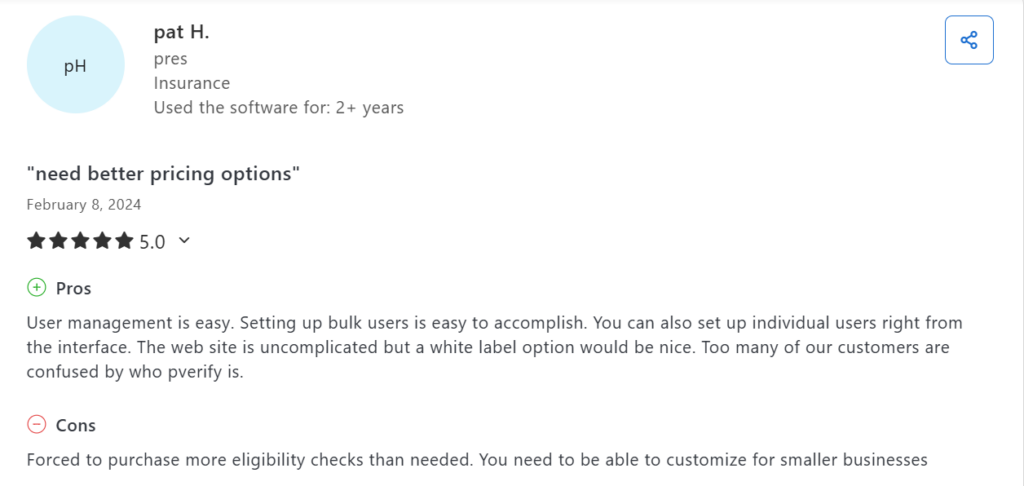
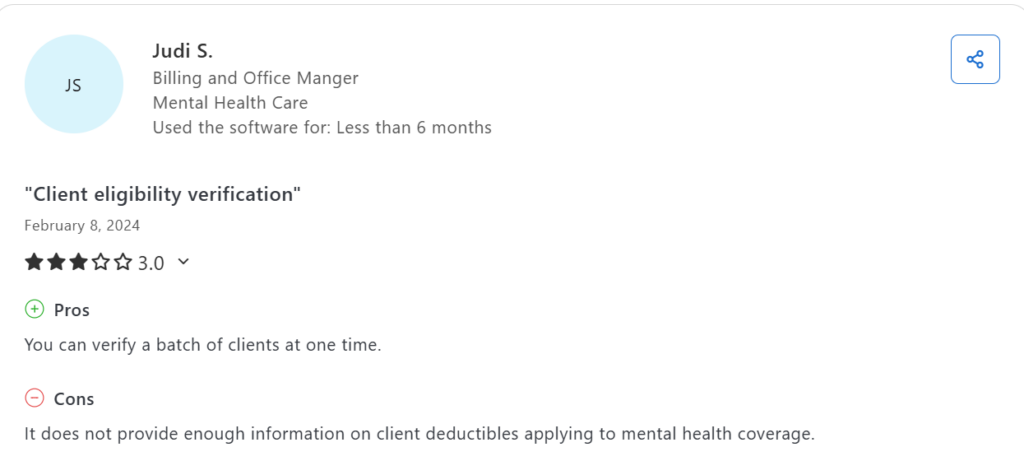
That answer depends on how your organization operates.
pVerify works well for:
In environments where eligibility is one component of a broader medical billing ecosystem, pVerify can function effectively.
pVerify is not built specifically for:
Behavioral health reimbursement introduces layers of nuance that go beyond confirming active coverage. Those nuances are tipping points that actively drive BH providers to search for alternatives.
Many behavioral health teams tend to start searching for alternatives when:
When these moments happen, it stops being a search for faster automation. It becomes a search for the right fit — a platform built around how behavioral health reimbursement actually works.
VerifyTreatment is a real-time insurance eligibility and RCM automation platform built specifically for behavioral health and mental health treatment centers. Not adapted from general medical billing, but built from the ground up for the payer logic and workflow complexity that BH providers deal with every day.

I demoed other platforms, and they were all medical-focused with limited behavioral health benefits. VerifyTreatment was the only one built specifically for inpatient psych and residential behavioral health. That’s what stood out—it was tailored to us.
.
Where pVerify gives you eligibility data, VerifyTreatment structures that data around the decisions your admissions and billing teams need to make. The result is fewer coverage surprises, cleaner handoffs, and stronger financial visibility from intake through reimbursement.
| Capability | pVerify | VerifyTreatment |
| Behavioral Health Specialization | Built for general healthcare providers across multiple specialties | Built specifically for behavioral health, SUD, and mental health workflows |
| Verification Depth | Real-time eligibility checks returning coverage data | Real-time VOB with BH-specific payer logic and structured summaries |
| Carve-Out & Authorization Logic | Requires manual interpretation of benefit data | Surfaces carve-outs, managed care nuances, and authorization indicators within workflow |
| Lapse Detection | Point-in-time eligibility checks | Automatic policy lapse detection and monitoring + payer alerts |
| Insurance Discovery | Coverage discovery using partial data | Advanced coverage discovery built for real-world BH intake scenarios |
| Payer Network | 1,000+ payers | 1,700+ payers with deep BH payer logic |
| Admissions-to-Billing Handoff | Eligibility exists separately from RCM workflows | Verification connects directly to billing and financial workflows |
| Workflow Integration | API-driven; integration dependent on internal setup | Salesforce/CRM-native integration designed for admissions teams |
| Pricing Structure | Modular, custom-quoted, variable by configuration | Transparent behavioral health–specific tiers |
| Implementation Experience | May require technical configuration | Fast deployment with BH-focused onboarding support |
pVerify earns its reputation. For multi-specialty medical groups and integration-heavy organizations that need modular eligibility infrastructure across general healthcare, it’s a capable, well-supported platform.
But for behavioral health providers scaling intake, expanding across multiple states, or actively fighting eligibility-driven denials, it can leave critical gaps. Behavioral health reimbursement carries payer nuances, carve-outs, and authorization requirements that VerifyTreatment is purpose-built for.
If your admissions team verifies on the first call and your billing team tracks eligibility-driven denials, it’s worth seeing how a purpose-built platform handles it differently.
pVerify can work for behavioral health organizations that run similarly to multi-specialty medical groups and don’t need BH-specific payer logic. But treatment centers managing SUD programs, Medicaid carve-outs, IOP authorizations, or multi-state expansion often find that general eligibility data leaves gaps that show up in denial rates and admissions conversion.
No. pVerify runs point-in-time eligibility checks. It doesn’t monitor policies continuously or flag coverage lapses between intake and admission. If your team needs proactive alerts before an inactive policy becomes a denied claim, that’s a gap worth factoring in.
VerifyTreatment is the strongest alternative for behavioral health treatment centers. It’s built specifically for SUD programs and mental health workflows, including carve-out logic, structured VOB summaries, lapse detection, and admissions-to-billing integration across 1,700+ payers.
pVerify connects to a broad payer network and can return eligibility data for many commercial and government plans. However, behavioral health providers should evaluate whether the returned data is structured in a way that supports Medicaid carve-outs, managed care nuances, and authorization requirements specific to their programs.
Usually because workflow gaps start hitting admissions and revenue.
Rising eligibility-driven denials, coverage surprises that delay or kill admissions, expansion into new states, and staff burnout from portal fatigue are the most common triggers. At that point, teams stop looking for faster automation and start looking for a platform built around behavioral health workflows.
Disclaimer: All trademarks, logos, and brand names are the property of their respective owners. The use of any third-party trademarks, logos, or brand names in this article is for informational and comparative purposes only, and constitutes nominative fair use. This article was published by VerifyTreatment, and while we strive for objective comparisons, VerifyTreatment is included as an option within this list.


Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.