
pVerify offers modular pricing, with eligibility starting around $125/month (500 transactions) and higher tiers near $395/month for 1,500 transactions. Additional tools like Insurance Discovery, MBI lookup, and other modules add $40–$150+ per month, so total costs rise with volume and features.
While pricing is transparent at the entry level, organizations that need fast, admissions-ready coverage detail may prefer a purpose-built option like VerifyTreatment.
Admissions and billing teams often lose time waiting on payer responses or rechecking coverage when patient information is incomplete.
pVerify helps reduce that manual work by offering real-time eligibility and insurance discovery through a web portal, APIs, and batch tools. Entry pricing is relatively transparent, but total costs tend to rise as you add modules, integrations, or higher transaction volume.
Below, we break down how pVerify pricing works, what you get at each level, where costs can add up, and when a behavioral health–focused alternative may be a better fit.
We work with treatment centers and multi-location providers that depend on fast, accurate eligibility decisions. With 4,000+ organizations on our platform and connections to 1,700+ payer databases, our view comes from real intake and revenue workflows, not just feature comparisons.

“Great Product, Ease of Use, Added Efficiency for Our Team. Automating and bringing in health insurance verifications to our instance was a game changer. We have instant verifications for all of our prospects, as well as automated verifications for our clients on a weekly basis.”
You can book a free demo today.
pVerify uses a modular pricing model based on transaction volume. Each feature is sold separately, with Standard and Enterprise tiers that increase as usage grows.

Core modules and starting ranges (annual contracts):
Additional tools, such as patient responsibility estimates, analytics, APIs, claims, or ERA services, are priced separately.
In practice, most organizations use multiple modules. Even modest add-ons (often $40–$150 per month each) can push total costs higher as needs grow. The model offers flexibility, but the more features and volume you add, the more the monthly spend increases.
pVerify is built to handle eligibility and coverage verification with tools that work for both day-to-day checks and higher-volume billing workflows. It covers the core tasks most teams rely on, with flexible ways to access and use the data.

Core capabilities include:
One thing many teams like about pVerify is the transparency. Starting prices are published, which makes early planning easier than with vendors that only provide custom quotes. The modular structure also keeps things flexible. You can start with core eligibility and add features over time as your volume or workflow needs grow.
The platform is also fairly easy to work with. Most users find the interface straightforward, and eligibility checks can be run quickly without a lot of training.
For billing teams or IT groups that need dependable eligibility data and solid integration options, pVerify fits well. It’s most commonly used to support claims and revenue workflows after patient information is already in place, rather than real-time decisions during intake.
pVerify is a solid eligibility tool, but there are a few limitations to keep in mind as your needs grow.
The entry price is modest, but expenses increase as you add modules or move into higher transaction tiers.
Once multiple features and higher volumes are in place, many organizations end up spending roughly $2,000–$12,000+ per year. For growing programs, the verification budget can climb faster than expected.
pVerify focuses on eligibility, not the full admissions or financial workflow. Features like patient estimates, claims follow-up, or workflow management sit in separate modules or other systems. Many teams end up working across multiple platforms or adding manual steps to fill the gaps.
The platform confirms coverage, but it doesn’t guide admissions conversations or highlight risk during the first call. Staff may still need to interpret benefits, check details, or follow up with payers, especially for behavioral health scenarios where coverage rules are more nuanced.
Core functionality centers on eligibility data. Patient responsibility estimates, deeper financial insight, or denial tracking typically require additional tools or upgrades.
Because pVerify is commonly used by billing teams, the information doesn’t always flow directly into admissions workflows or CRM systems. This can leave front-end staff and back-office teams working from different sources.
Overall, pVerify provides reliable eligibility building blocks, but turning those pieces into a complete front-end workflow often takes additional tools, integrations, or manual coordination.
For organizations that need fast financial clarity during intake, that extra complexity can become part of the day-to-day workload.
For organizations that need clear insurance answers during intake, VerifyTreatment is built around how behavioral health admissions actually work.
Our platform brings key tasks into one place, like real-time eligibility, insurance discovery, payer alerts, claim visibility, and CRM/EHR integration, so teams don’t have to piece together multiple tools.
The platform focuses on the moment when decisions are being made. During the intake call, it returns detailed coverage information such as level-of-care limits, authorization requirements, deductibles, and estimated patient responsibility, instead of a simple active/inactive response.
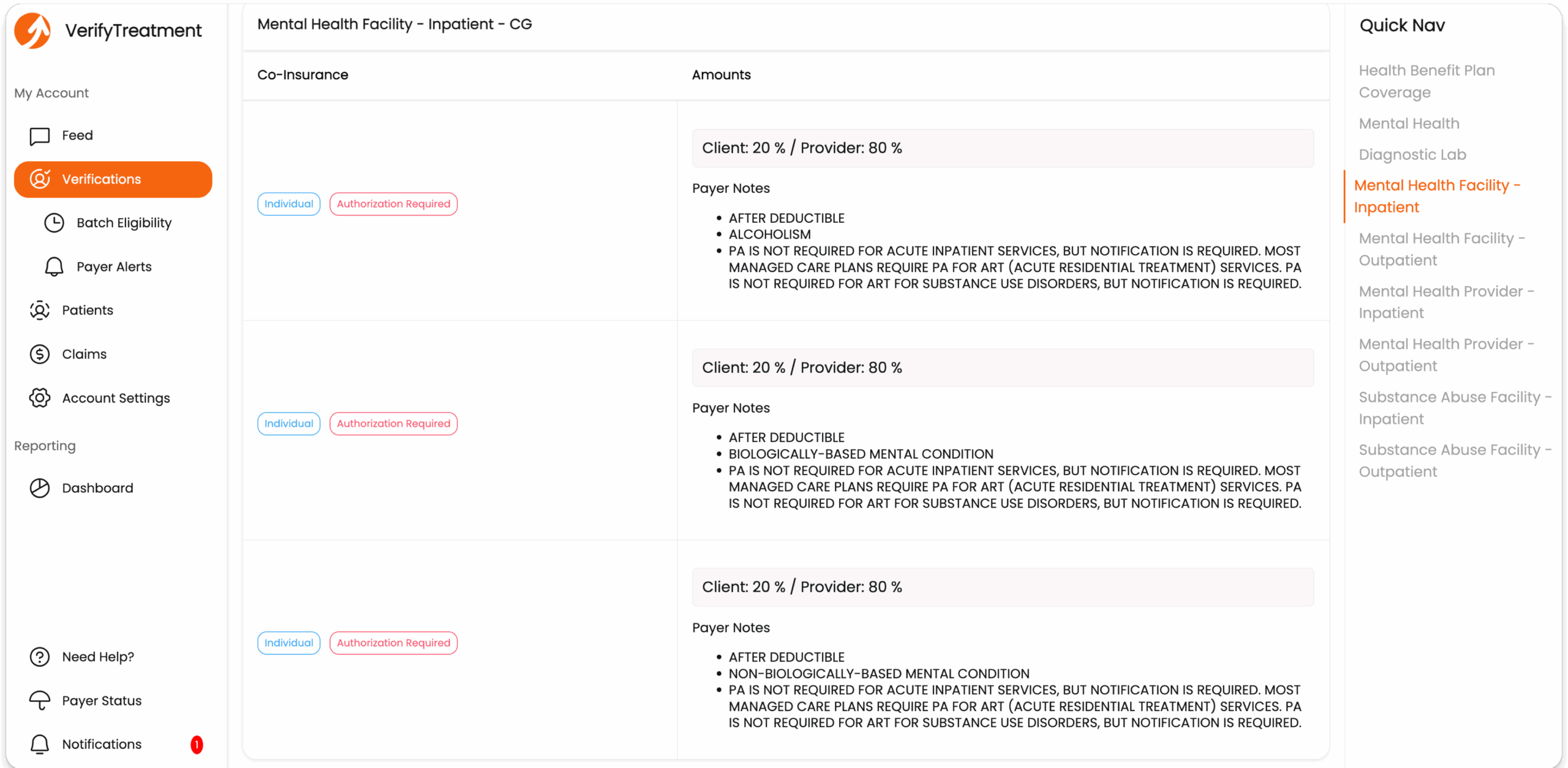
If information is incomplete, insurance discovery can often locate active coverage using basic details like name and date of birth, helping teams move forward without delays.
Support doesn’t stop after the first check. VerifyTreatment can flag policy changes or lapses and provide claim status visibility so billing teams see potential issues earlier. Because the data flows directly into systems like Salesforce, admissions, utilization review, and billing teams all work from the same information without extra data entry or portal switching.
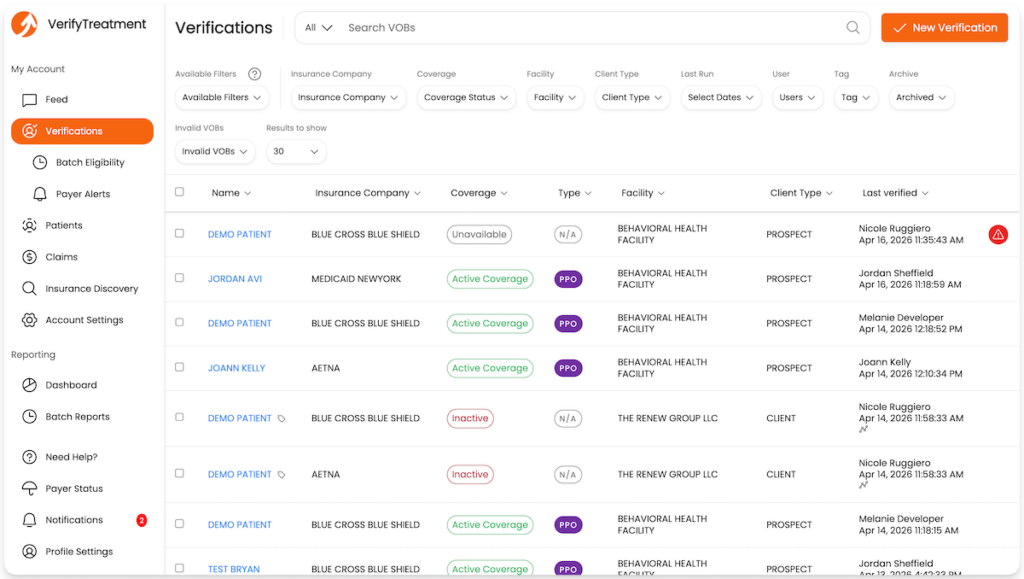
Key capabilities include:
For behavioral health teams, the value is simple: clearer coverage information earlier in the process and fewer surprises as patients move from admissions to billing.
To be clear, VerifyTreatment was built around the issues teams run into most—manual checks, unclear coverage, and gaps between admissions and billing.
Our platform was designed around behavioral health workflows, not adapted from general medical billing.
It recognizes common payer nuances such as mental health carve-outs, level-of-care limits, managed Medicaid rules, and plan variations, and presents the information in a way your admissions team can use without extra research or follow-up calls.
We bring eligibility, insurance discovery, claim visibility, and payer alerts into one system. Instead of stacking separate modules or vendors, your team works from a single workflow, which helps reduce complexity and ongoing integration work.
Verification results flow into the same system used by admissions and billing, so everyone works from the same information. This helps reduce handoff gaps and makes it easier to catch issues earlier.
More detailed eligibility checks and ongoing monitoring help surface authorization needs, coverage changes, or policy lapses sooner. Addressing these details earlier can help reduce downstream rework and unexpected claim issues.
We designed the platform to be practical and easy to use, with a modern interface and a setup process that helps teams get up and running quickly.
In short, VerifyTreatment brings insurance verification closer to the intake process, so your team has clearer information earlier without adding more tools or manual steps.
pVerify gives you flexible building blocks for eligibility, but many teams still end up managing separate tools and workflows. VerifyTreatment brings those pieces together into one admissions-focused experience, including:
If your team needs clearer answers earlier in the process, a short demo is the easiest way to see how it works in real situations. Get started today.
Disclaimer: All trademarks, logos, and brand names are the property of their respective owners. The use of any third-party trademarks, logos, or brand names in this article is for informational and comparative purposes only, and constitutes nominative fair use. This article was published by VerifyTreatment, and while we strive for objective comparisons, VerifyTreatment is included as an option within this list.


Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.