
Insurance verification software checks active coverage and benefits in real time, giving your team clear answers without payer-portal logins or long calls. This guide outlines the top tools for 2026, from real-time eligibility engines to API platforms and full RCM systems with built-in verification.
| Tool | Best for |
|---|---|
| VerifyTreatment | Best for behavioral-health admissions |
| Waystar | Best for enterprise coverage detection |
| Eligible | Best developer/API-first option |
Insurance checks should be simple, but many teams still jump between payer portals, wait on hold, and piece together benefits from several sources. That slow process often leads to missing details, confused coverage questions, and admissions that stall while everyone waits for answers.
Modern insurance verification software fixes this by pulling accurate coverage data in real time. You get plan type, benefits, co-pays, deductibles, and limits within seconds. Many tools also flag policy changes so your team works with current information instead of chasing updates later.
The platforms below offer faster intake and cleaner billing workflows, giving teams a steadier way to confirm coverage from the first step.
At Verify Treatment, we built our platform to solve the problems we kept seeing across treatment centers, from missed admissions, stretched staff, to denials tied to avoidable coverage issues.
“Great Product, Ease of Use, Added Efficiency for Our Team. Automating and bringing in health insurance verifications to our instance was a game changer. We have instant verifications for all of our prospects, as well as automated verifications for our clients on a weekly basis.”

“The product is lightning fast, and so easy to use. In terms of instant verification, there is nothing faster or more comprehensive in my experience. Highly recommend for billing and admissions departments.”

Today, more than 4,000 behavioral health providers rely on our platform to verify benefits and support their admissions and billing teams. That day-to-day experience gives us a clear view of what actually works, what doesn’t, and which features make a difference when time and accuracy matter.
Below is a breakdown of each option so you can see which one fits your workflow.
| Tool | Real-time eligibility | Discovery | BH focus | Prior auth | Batch checks | Integrations | Pricing |
|---|---|---|---|---|---|---|---|
| VerifyTreatment | ✅ Yes | ✅ Yes | ✅ Yes | ⚠️ Limited | ✅ Yes | CRM / EHR | Quote-based |
| Myndshft | ✅ Yes | ✅ Yes | ⚠️ Partial | ✅ Yes | ✅ Yes | API / EHR | Quote-based |
| pVerify | ✅ Yes | ✅ Yes | ❌ No | ⚠️ Limited | ✅ Yes | API / EDI | Tiered |
| Waystar | ✅ Yes | ✅ Yes | ❌ No | ✅ Yes | ✅ Yes | Deep EHR / Clearinghouse | Enterprise |
| Availity | ✅ Yes | ⚠️ Partial | ❌ No | ✅ Yes | ✅ Yes | Portal / APIs | Free tier + paid |
| Eligible | ✅ Yes | ⚠️ Partial | ❌ No | ⚠️ Some | ✅ Yes | REST / FHIR APIs | Per-call |
| InstantVOB | ✅ Yes | ⚠️ Limited | ❌ No | ❌ No | ⚠️ Limited | Web / API | Monthly tiers |
| QuickAdmit | ✅ Yes | ✅ Yes | ✅ Yes | ⚠️ Limited | ✅ Yes | Intake / EHR connectors | Quote-based |
| Experian Health | ✅ Yes | ✅ Yes | ❌ No | ⚠️ Some | ✅ Yes | Suite APIs | Enterprise |
| Clearwave | ✅ Yes | ⚠️ Partial | ❌ No | ❌ No | ✅ Yes | Registration / EHR | Subscription |
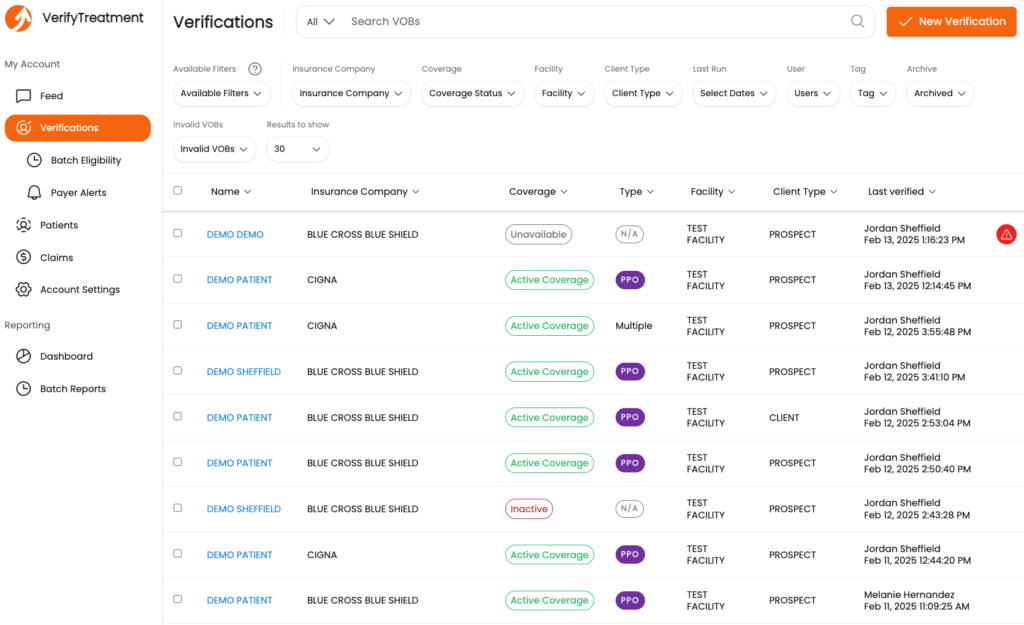
We built VerifyTreatment for the daily pressures inside behavioral health admissions. Many platforms serve broad medical use, but ours focuses on mental health and SUD programs that work with:
When a new inquiry comes in, our platform checks coverage with more than 1,700 payers and returns a full benefit picture in seconds. Teams see deductibles, co-pays, benefit limits, and authorization details without moving through multiple portals or waiting on calls.
VerifyTreatment also re-checks benefits for pending clients through nightly batch runs. This helps teams catch policy changes early and reduces issues that appear later in billing.
Our CRM integrations, including Salesforce, and connections to behavioral health EHRs let admissions and billing teams work from the same information without repeating work.
QuickAdmit focuses on admissions teams that need fast benefit checks at any hour. The platform connects to a wide range of commercial payers through single sign-on, which helps staff pull coverage details without moving through several portals.
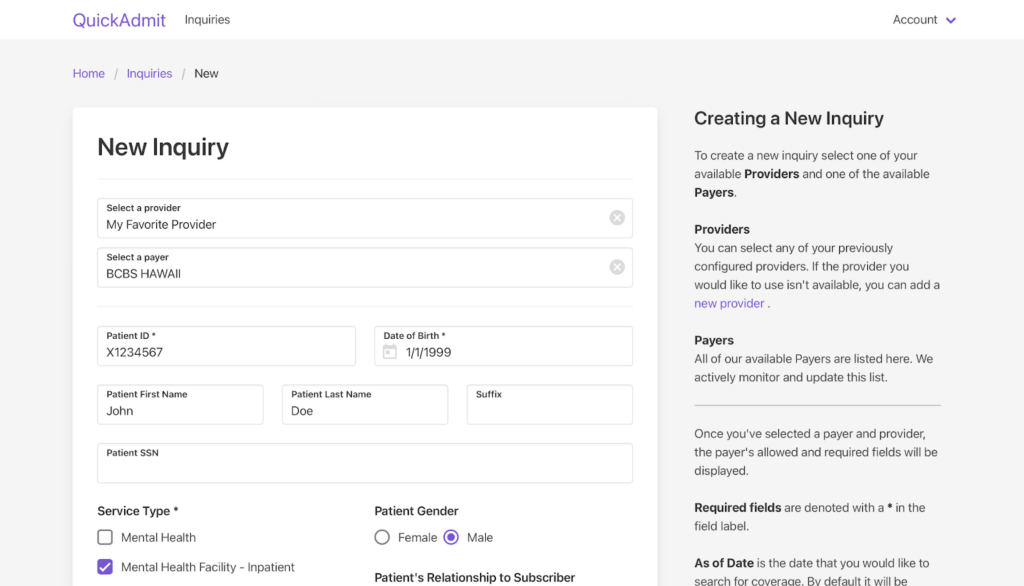
Teams enter basic patient information and receive a VOB report within seconds, including evenings and weekends. The mobile-friendly layout supports programs that receive many after-hours inquiries, which is common in behavioral health and substance use treatment.
QuickAdmit also checks for active coverage across multiple data sources at the same time. This helps staff confirm benefits even when callers have limited or incomplete insurance details.
$285 Starter Plan
Availity runs one of the largest health information networks in the country, giving providers real-time eligibility across Medicaid, Medicare, and commercial plans.

Many small practices start with the free Essentials portal for basic checks, while larger organizations move to Essentials Plus or Pro for broader payer access, batch runs, and EHR-connected workflows.
Hospitals and clinics often use Availity as a central entry point for eligibility, prior authorization, and other financial functions because it ties together many payers in one place.
Waystar offers automated eligibility checks and a tool that finds active insurance coverage without manual searches. It connects to many payers and can identify primary or secondary policies even when you only have limited patient details. When new information is added, Waystar runs another check and updates the record so teams always see current coverage.
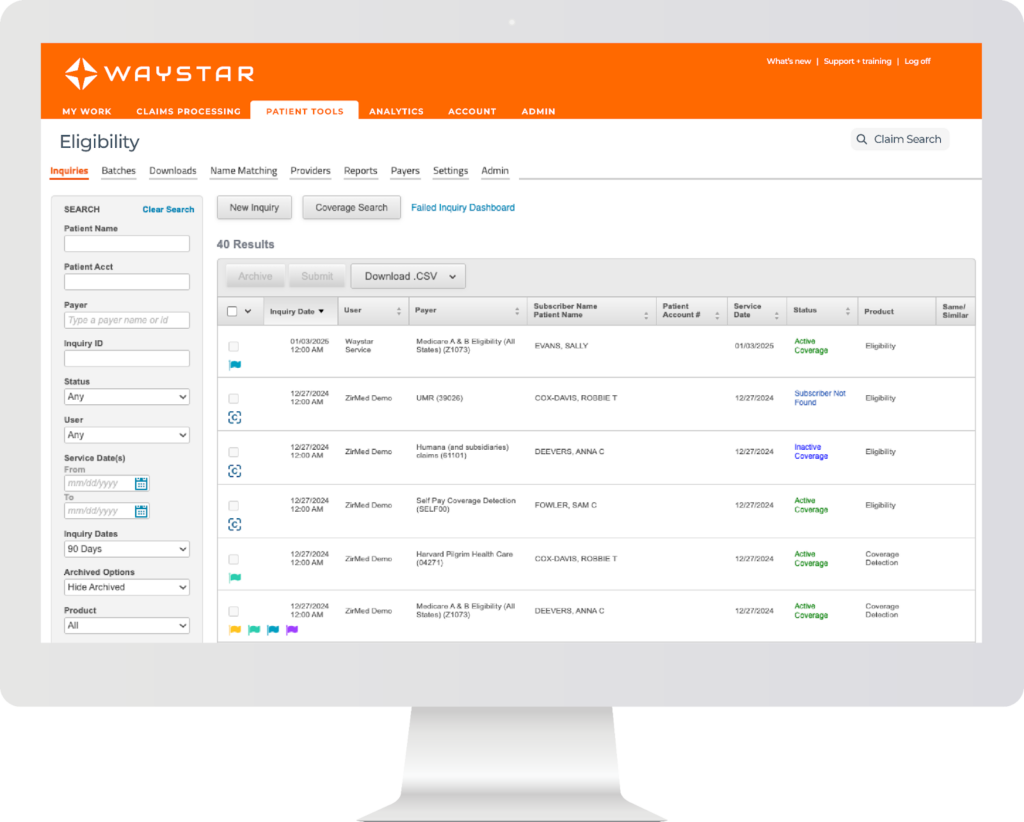
The platform links to major EHRs and reduces the need to log into payer portals or track down missing insurance data, which helps staff work more efficiently.
Experian Health provides an eligibility system that connects to a large national payer network through a high-availability clearinghouse. Many hospitals and large clinics use it because the platform standardizes payer responses and blends data from multiple sources, giving staff clearer benefit details.

It can also pull Medicare Beneficiary Identifiers and coordination-of-benefits data from CAQH, which helps teams identify the correct primary coverage early in the intake process. The system is often part of Experian’s larger patient-access suite, which includes scheduling, financial tools, and other front-office support.
pVerify (by DoseSpot) provides real-time eligibility checks through a web portal, batch tools, or API connections. It reaches a wide network of medical, dental, and vision payers and lets organizations automate verification steps through a rules engine.

Teams can set triggers to check certain plans or run verifications on a schedule, which helps reduce manual work. The system returns detailed benefits, such as deductibles, co-pays, and limits, and can show when a plan may need prior authorization. It also offers claims-history lookup, giving billing teams added context before submission.
These features support programs that want clear benefit information early in the workflow so admissions and billing staff can move cases forward with fewer delays.

Eligible is a developer-focused insurance and billing API used by digital health companies, telehealth apps, and modern clinics.

Instead of relying on portals, teams can verify coverage, pull benefit details, estimate patient costs, and submit claims through simple API calls. This lets organizations build their own user interfaces, such as patient portals, mobile apps, or intake tools, while Eligible handles the complex data work behind the scenes.

InstantVOB is a simple, cloud-based tool for providers that need quick benefit checks without a long setup process. Staff enter basic patient information through the portal or a web form on the clinic’s site, and the system returns a VOB report in seconds.
The report includes active status, deductibles, out-of-pocket amounts, co-pays, specialty coverage, and available demographics.
The platform is mobile-friendly, so teams can run checks from a phone or tablet, which helps smaller practices or staff working in the field. Because it operates around the clock, admissions teams can verify coverage during evenings or weekends without relying on payer portals.

Myndshft is an automation platform built to handle detailed patient-access tasks. It began with prior authorization and later added eligibility checks, insurance discovery, coordination of benefits, and patient cost estimates.

Instead of requiring staff to move through multiple payer portals, the system uses automation to pull information from several sources and present it in one place. This helps teams find active insurance even when patient details are limited.
The system can re-run verifications in the background and send alerts when coverage information changes. Because the platform supports both medical and pharmacy authorization workflows, larger organizations often use it to manage many moving parts across intake, authorization, and billing.
Clearwave checks eligibility several times during the patient visit instead of relying on a single lookup. The system runs eligibility at scheduling, pre-check, check-in, and after the visit.
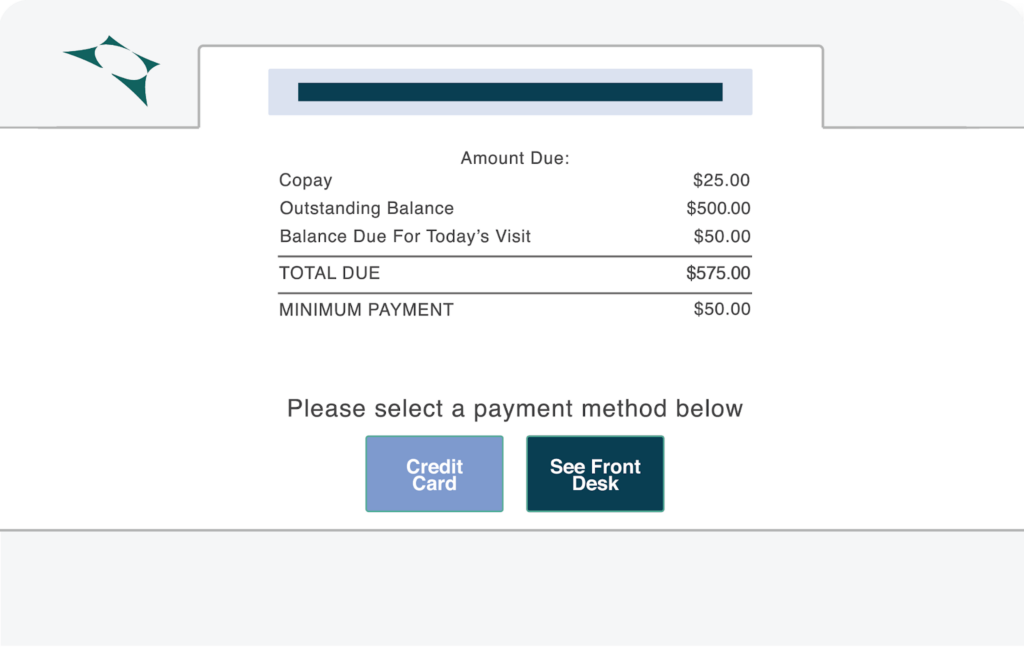
This matters because insurance details can shift between booking an appointment and arriving in the office, and those changes often lead to unexpected denials.
Clearwave pulls data from clearinghouses and payer APIs, updates plan details automatically, and flags issues when a patient’s insurance no longer matches payer records.
For front-desk teams, this means more accurate co-pay and deductible collection. For billing, it means fewer follow-up calls and fewer claims stalled by outdated information.
VerifyTreatment gives behavioral health programs real-time coverage detail, deep payer logic, and automated checks designed for the way treatment centers operate. More than 4,000 providers use our platform because it focuses on behavioral health workflows—not generic medical tools—and delivers a complete benefit picture in seconds.
If you want faster intake and fewer eligibility issues, book a quick demo and see how VerifyTreatment supports your staff from the first call onward.
Insurance verification software checks a patient’s active coverage and benefits in real time. Staff enter basic details, and the system returns plan status, co-pays, deductibles, limits, and any requirements.
Many tools also flag policy changes or find missing insurance, giving teams clear information before they move forward.
The right choice depends on your volume, payer mix, and workflow. For behavioral health, VerifyTreatment is a strong fit because it delivers real-time eligibility, detailed payer logic, and high-volume batch checks.
Start with your main bottleneck, like slow intake, eligibility issues, or manual prior authorization steps. Then compare vendors on payer reach, integration options, speed, and total operating costs.
Most facilities look for real-time eligibility, insurance discovery from partial data, batch checks, lapse alerts, claim-status and ERA visibility, and simple EHR or CRM integration.
VerifyTreatment uses detailed payer logic, insurance discovery, and lapse alerts so admissions teams get a full benefit picture on the first call. This helps staff catch issues early and move cases forward with fewer eligibility problems.
Yes. VerifyTreatment offers Salesforce integration, API options, and batch tools that support multi-location and multi-state programs without adding extra manual work.
Teams often see faster first-call verifications, less time in payer portals, and fewer eligibility-related denials. Many customers say eligibility is a major driver of their denials, and automation helps reduce that burden.
Disclaimer: All trademarks, logos, and brand names are the property of their respective owners. The use of any third-party trademarks, logos, or brand names in this article is for informational and comparative purposes only, and constitutes nominative fair use. This article was published by VerifyTreatment, and while we strive for objective comparisons, VerifyTreatment is included as an option within this list.



Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.