
Choosing the right behavioral health revenue cycle management (RCM) partner depends on where revenue breaks down in your operation. Some organizations need full-service billing, others require enterprise-level reporting, while many struggle earlier at intake, eligibility, and authorization. This guide reviews the 9 leading behavioral health RCM companies, outlining how each approaches billing, prevention, automation, and financial visibility. This way, you can match the right solution to your organization’s size, complexity, and revenue risk profile.
| Tool | RCM Focus Area | Best for |
|---|---|---|
| VerifyTreatment | Front-end revenue protection (intake & eligibility) | Practices losing revenue to denials before claims |
| Lightning Step | Best for enterprise coverage deEnd-to-end platform (EHR + CRM + RCM) | Mid-to-large treatment centers and enterprises |
| Kipu | Enterprise-scale, full-cycle RCM | Large, multi-facility behavioral health systems |
Finding the right behavioral health RCM partner can be exhausting. Most options fall into one of two camps: general medical billing companies that don’t understand behavioral health nuances, or “all-in-one” platforms that promise simplicity but deliver manual setup, weak reporting, and inconsistent support.
And even when you finally choose, the real issues often surface later — denied claims, limited AR visibility, credentialing gaps, and support teams that can’t explain why things break. To save you months of trial and revenue leakage, we curated a list of the 9 best behavioral health RCM companies based on real-world fit and performance.
We work closely with admissions, billing, and RCM teams across thousands of behavioral health organizations, giving us firsthand insight into where revenue is lost before billing begins. VerifyTreatment was built to address front-end breakdowns like incomplete verification, missed authorizations, and poor handoffs.
Here’s what a VerifyTreatment user had to say:
“Great Product, Ease of Use, Added Efficiency for Our Team. Automating and bringing in health insurance verifications to our instance was a game changer. We have instant verifications for all of our prospects, as well as automated verifications for our clients on a weekly basis.”

“The product is lightning fast, and so easy to use. In terms of instant verification, there is nothing faster or more comprehensive in my experience. Highly recommend for billing and admissions departments.”

Behavioral health revenue cycle challenges are rarely caused by billing alone. Most issues originate earlier in the workflow and compound as patients move from intake to care to claims.
Many tools confirm active coverage but fail to surface behavioral health carve-outs, authorization requirements, visit limits, or benefit exhaustion. These gaps often aren’t discovered until claims are denied and too late to fix.
Manual verification workflows slow intake. While teams wait on portals or payer calls, qualified patients may choose faster providers, leading to empty beds and lost revenue.
Critical information verified during intake doesn’t always reach billing or clinical teams. When exclusions, limits, or payer quirks aren’t communicated, claims are submitted with missing or incorrect context.
Many practices lack clear insight into:
Without this visibility, teams are forced into reactive cleanup instead of proactive revenue protection.
As inquiry volume increases, manual processes limit how many patients teams can safely verify and admit each day—capping growth even when demand is strong..
Many of the most common behavioral health RCM challenges are now solvable with the right mix of tools and expertise. Below is a quick glance at the top behavioral health RCM companies in 2026 and how they approach revenue protection, billing, and scale.
Below is a breakdown of each option so you can see which one fits your workflow.
| Company | RCM Model | Primary Focus Area | How Revenue Is Protected | Best Fit For |
| VerifyTreatment | Pre-billing intelligence platform | Eligibility, carve-outs, authorizations | Prevents denials before admission by surfacing coverage risks early | Organizations losing revenue at intake or admissions |
| Lightning Step | All-in-one platform (EHR + CRM + RCM) | Admissions → clinical → billing continuity | Reduces billing errors through unified workflows and AI-assisted documentation | Mid-to-large treatment centers seeking one system |
| Kipu | Enterprise EHR with embedded RCM | High-volume billing & reporting | Improves clean claim rates and AR visibility through deep EMR integration | Large, multi-facility behavioral health organizations |
| Global Healthcare Resource | Fully outsourced RCM service | End-to-end billing execution | Eliminates internal billing overhead with dedicated billing teams | Practices that want to offload billing entirely |
| Behave Health | Lightweight all-in-one software | Ease of use & fast adoption | Simplifies billing and collections inside one system | New or growing programs prioritizing simplicity |
| Cantata Health | Enterprise financial & RCM platform | Financial oversight & analytics | Uses predictive analytics and GL-level controls to reduce leakage | Complex organizations with centralized business offices |
| SmartCare™ (Streamline Health) | EHR-embedded RCM | Clinical-driven billing accuracy | Validates charges against documentation before claims submission | Behavioral health & human services organizations |
| Med USA | Managed RCM & credentialing services | Billing + payer enrollment | Closes reimbursement gaps caused by credentialing & compliance issues | Practices struggling with payer enrollment & AR |
| AxiomEHR | Analytics-driven RCM within EHR | Financial visibility & denial reduction | Highlights friction points with real-time analytics and automation | Teams needing insight into why revenue is delayed |
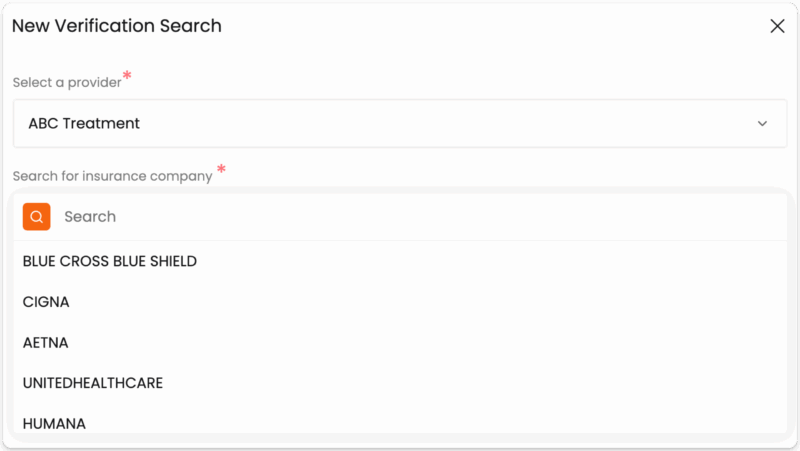
VerifyTreatment addresses one of the most costly breakdowns in behavioral health RCM: coverage issues that aren’t identified until after care has already been delivered. When exclusions, authorization requirements, or benefit limits are missed at intake, downstream denials are often unavoidable.
Unlike traditional RCM solutions that focus on fixing problems after claims are submitted, VerifyTreatment concentrates on preventing those problems upfront. It combines real-time eligibility verification, payer-specific intelligence, and active policy monitoring to surface risk early and support faster, more confident admissions.
In practice, this approach delivers measurable results. Foundations Recovery Network reduced admissions delays, lowered staffing strain, and prevented the loss of 1 in 10 patients, saving over $10,000 per month in avoidable revenue loss after implementing VerifyTreatment.
Behavioral health practices and facilities that want to prevent denials, accelerate admissions, and protect revenue before billing and claims submission.

“Great Product, Ease of Use, Added Efficiency for Our Team. Automating and bringing in health insurance verifications to our instance was a game changer. We have instant verifications for all of our prospects, as well as automated verifications for our clients on a weekly basis.”
Lightning Step treats revenue cycle management as one of its three core pillars, alongside EHR/EMR and CRM, making it an all-in-one platform built specifically for behavioral health organizations.
Rather than separating admissions, clinical documentation, and billing into disconnected systems, Lightning Step brings these functions into a single workflow, from inquiry and intake through treatment and reimbursement.
This approach aligns with user feedback shared publicly by behavioral health operators. In one Reddit discussion comparing EHR and RCM platforms, a provider who transitioned from InSync described Lightning Step as “a game changer,” citing its more modern interface, direct clearinghouse connections, and built-in AI tools for clinical notes as meaningful improvements over legacy systems.
Mid-to-large behavioral health organizations and treatment centers that want a single platform to manage admissions, clinical care, billing, and revenue cycle operations in one place.
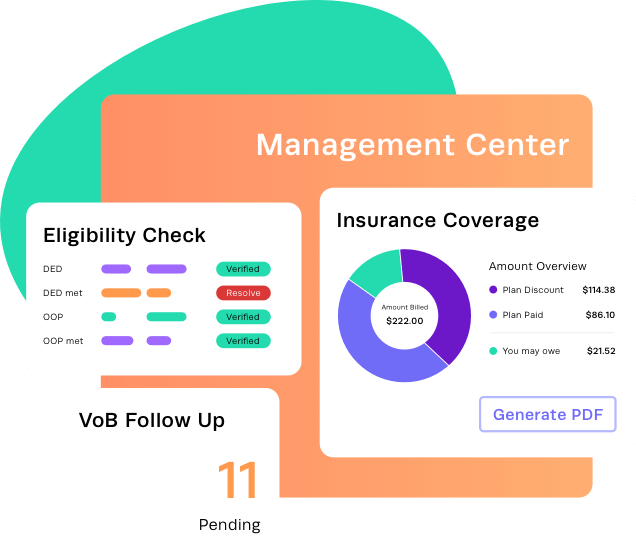
Kipu positions revenue cycle management as part of a broad, enterprise-grade platform that combines EMR, CRM, RCM, and compliance management for behavioral health organizations.
Its RCM capabilities are tightly integrated with clinical and operational workflows, allowing teams to manage eligibility, authorizations, claims, patient billing, and reporting from a single system.
Across user feedback, Kipu is often described as comprehensive and easy to navigate for its size, with strong visibility into both patient and financial data. Billing teams frequently point to its reporting and claims transparency, especially the ability to export data for deeper analysis as key strengths.
At the same time, users note trade-offs like higher costs as organizations scale, superuser-dependent controls, and eligibility details that may feel less granular than specialized tools.
Large behavioral health organizations and enterprise treatment centers that need a full-scale RCM system capable of handling high volume, complex billing, and multi-location operations.
Global Healthcare Resource offers outsourced revenue cycle management services for behavioral health organizations that prefer to offload billing, coding, and accounts receivable operations entirely.
Rather than providing software, Global builds dedicated teams of billing, coding, and call center professionals that operate as an extension of a client’s internal staff.
Behavioral health practices and facilities that want to fully outsource billing and revenue cycle operations, especially those without dedicated in-house billing teams.

Behave Health aims to make revenue cycle management easier to operate for behavioral health organizations by reducing the number of systems required to run day-to-day operations. The platform combines EHR, CRM, ERP, and RCM to give providers a single system for managing admissions, documentation, billing, and operational workflows.
This emphasis on ease of use is reflected in customer feedback. On Capterra, administrators frequently describe Behave Health as intuitive and straightforward. As one Outreach Director puts it, “BehaveHealth is very user friendly. The customer service experience is incredible.”
That said, some users also note trade-offs common to lighter-weight platforms, including an initial learning curve during setup and occasional performance slowdowns when moving between features.
New or growing behavioral health organizations, recovery residences, sober living programs, and treatment centers that want an easy-to-use all-in-one platform with built-in RCM capabilities.

Cantata Health approaches revenue cycle management as part of a broader financial and operational platform rather than a standalone billing tool. Built on its Arize Platform, Cantata combines RCM, financial management, cost accounting, and operational software to support behavioral health and acute care organizations with complex business and reporting needs.
Its RCM capabilities are tightly integrated with general ledger routing, predictive analytics, contract management, and eligibility workflows, making it well suited for organizations operating centralized business offices.
Cantata’s platform has also been recognized at the industry level. Black Book Research awarded Cantata Highest Client Satisfaction for Revenue Cycle Management, Client Accounting, and Enterprise Resource Planning software.
Large behavioral health organizations, health systems, and multi-facility providers that require robust financial oversight, advanced reporting, and a centralized approach to revenue and operational management.
SmartCare™ RCM is the revenue cycle management solution within the SmartCare EHR platform, developed by Streamline Health. Like Lightning Step, SmartCare™ RCM is designed to work directly off clinical documentation rather than operating as a separate billing system. This makes it particularly useful for behavioral health and human services organizations where billing accuracy depends heavily on timely and complete clinical records.
Even though there is limited RCM-specific user feedback, reviews of the broader SmartCare EHR on Software Finder offer relevant insight. Users frequently highlight strong billing functionality, intuitive clinical views, and efficient reporting across financial and care data.
On the flip side, some users point out gaps in accounting exports and financial tooling at scale, suggesting SmartCare™ RCM is best suited for organizations that prioritize clinical-billing alignment over enterprise-grade financial systems.
Behavioral health and human services organizations that want tight integration between clinical documentation and billing, particularly those managing complex reimbursement rules without needing a full enterprise financial platform.
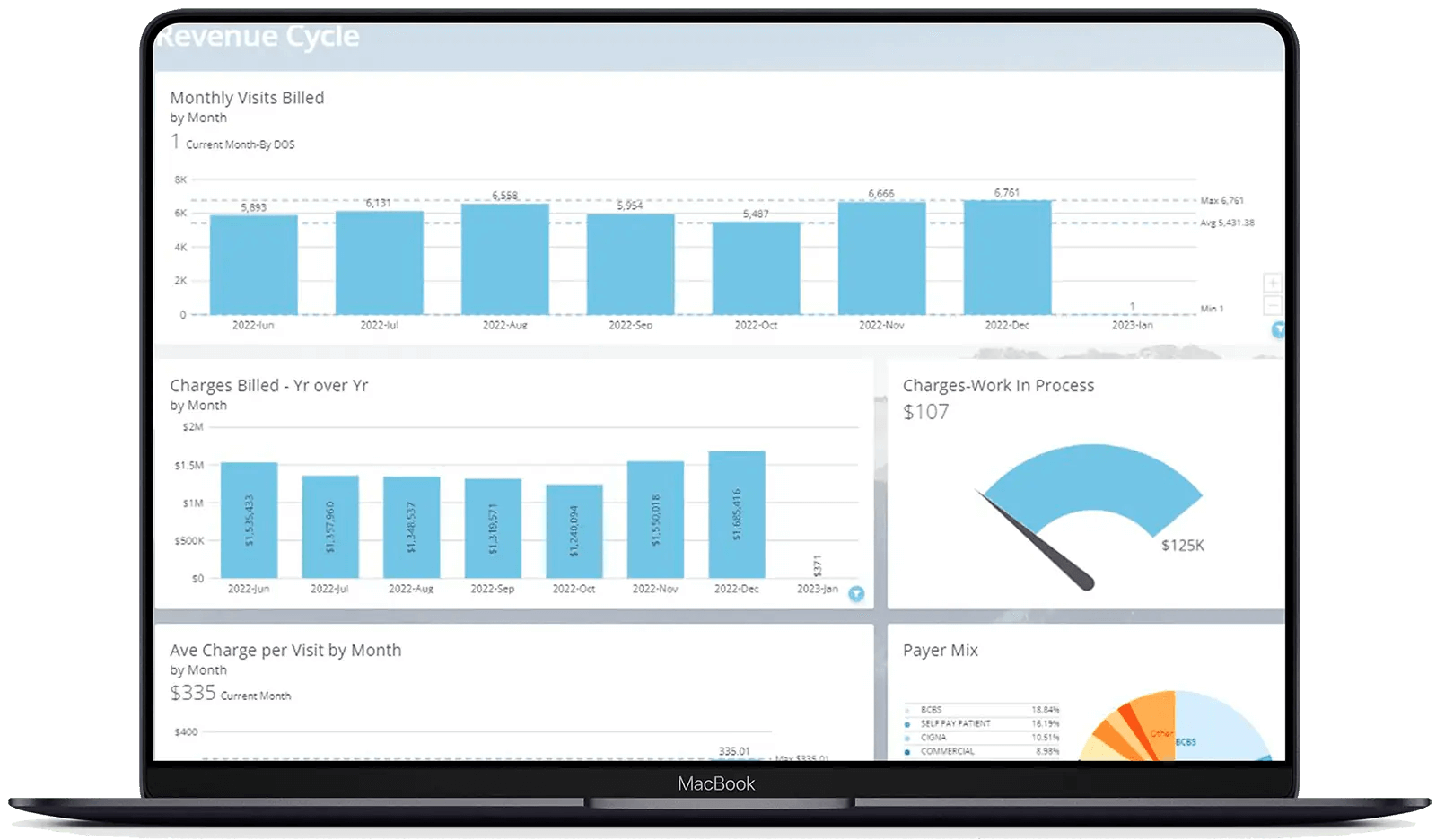
Med USA approaches revenue cycle management as a fully managed service rather than a software platform. In practice, that means behavioral health providers outsource the most complex parts of billing, credentialing, and compliance to a dedicated team instead of relying on internal staff or learning new systems.
The company specializes in behavioral health billing and credentialing, addressing common cash-flow blockers such as payer enrollment delays, credentialing gaps, compliance risk, and reimbursement friction unique to mental health services.
Behavioral health practices and mental health providers that want to outsource billing, credentialing, and compliance while maintaining visibility into performance.
AxiomEHR offers a revenue cycle management experience focused on financial clarity rather than volume processing. The platform emphasizes real-time visibility into denials, rework, payer friction, and revenue trends, helping behavioral health teams understand where money is delayed or lost across the billing cycle.
Behavioral health organizations that want analytics-driven, configurable RCM tightly integrated into their EHR rather than relying on external billing systems or fully outsourced services.
Behavioral health revenue cycle management doesn’t follow a single model. Some organizations need eligibility intelligence before admission, others need tightly integrated EHR billing, while some prefer fully outsourced billing and credentialing. Because of that, we did not evaluate vendors on feature count alone.
Instead, we focused on how each company addresses the specific breakdowns that cost behavioral health providers time, revenue, and operational confidence.
Our evaluation was based on the following criteria:
We looked at when in the patient and billing lifecycle each solution operates:
Platforms that clearly reduce risk at critical points scored higher than those that simply process claims.
We prioritized companies built specifically for behavioral health and human services, not general medical billing tools adapted later. This includes support for:
Not every organization wants the same level of ownership. We evaluated whether each solution supports:
Solutions were assessed on how clearly they define roles, visibility, and accountability.
Because billing accuracy in behavioral health depends heavily on documentation, we evaluated how closely RCM functions are tied to:
Tighter clinical-billing alignment was weighted heavily.
We assessed how well organizations can understand:
This includes dashboards, reporting depth, exportability, and real-time alerts.
Where available, we incorporated:
We did not assume performance where evidence was limited, and we called that out transparently.
Finally, we evaluated how each solution performs as organizations grow:
Every entry includes trade-offs, because no RCM solution is universally “best.”
The right behavioral health RCM company depends on where revenue breaks down in your organization. Some teams need full-cycle billing execution, others need enterprise-grade reporting, and many struggle much earlier—at intake, eligibility, and authorization where mistakes quietly turn into denials weeks later.
If your revenue issues start before a claim is ever submitted, prevention matters more than recovery. That’s where VerifyTreatment stands apart by identifying coverage risks upfront so admissions decisions are made with clarity.
Get Started with VerifyTreatment Here
Behavioral health revenue cycle management (RCM) includes all processes that impact revenue from insurance verification and admissions to billing, claims, denials, and reimbursement. Because behavioral health has unique payer rules and authorization requirements, RCM in this space is often more complex than general medical billing.
Behavioral health RCM involves additional challenges such as carve-outs, visit limits, levels of care (IOP, PHP, inpatient), and stricter authorization requirements. Many general medical RCM tools don’t handle these nuances well, leading to preventable denials and revenue loss.
It depends on your practice. Some organizations prefer outsourced billing services to handle claims and AR, while others use RCM software to maintain more control in-house. Many behavioral health practices use a combination of tools—front-end verification, billing software, and external services—to cover gaps across the revenue cycle.
In most cases, no. Behavioral health practices often rely on multiple systems that address different parts of the revenue cycle. The most effective setups prioritize preventing errors early and ensuring clean handoffs between admissions, billing, and clinical teams.
Key factors include behavioral health expertise, denial prevention, workflow fit, reporting visibility, support quality, and scalability. The right solution should reduce manual work while improving revenue protection.
Disclaimer: All trademarks, logos, and brand names are the property of their respective owners. The use of any third-party trademarks, logos, or brand names in this article is for informational and comparative purposes only, and constitutes nominative fair use. This article was published by VerifyTreatment, and while we strive for objective comparisons, VerifyTreatment is included as an option within this list.



Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.