

TriZetto Provider Solutions is a long-time clearinghouse known for claims editing and broad payer reach, while Waystar offers a newer, cloud-based RCM platform with usage-based pricing.
That said, neither tool is built for behavioral health intake, where teams need quick answers on coverage details like carve-outs or level-of-care limits. For treatment centers that need clear eligibility on the first call and fewer surprises later, VerifyTreatment is often a better fit.
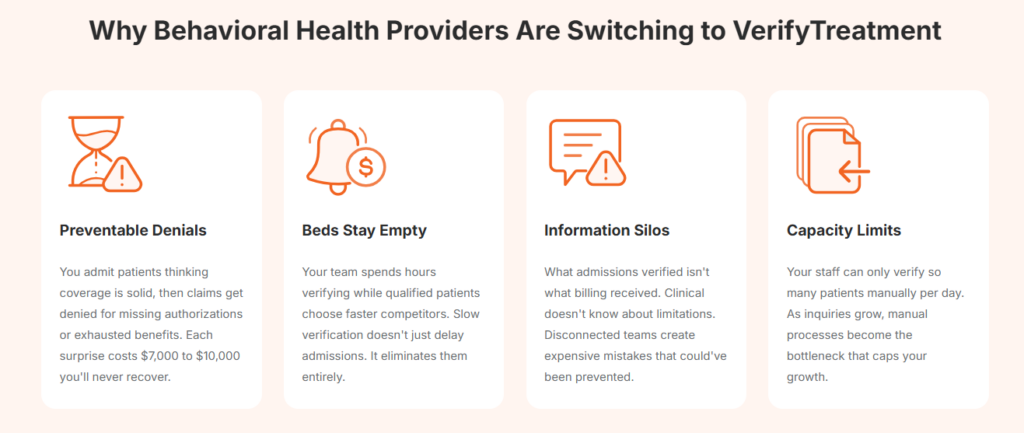
For behavioral health and addiction treatment centers, insurance checks often happen under time pressure. Admissions teams need clear answers while a prospective patient is still on the phone, and billing teams need fewer problems showing up days or weeks later.
Two platforms are commonly compared in this context: TriZetto Provider Solutions and Waystar. TriZetto is known for its long history as an enterprise clearinghouse, while Waystar emphasizes cloud-based automation across claims and RCM.
Below, we compare TriZetto and Waystar side by side, explain where each fits best, and outline why many behavioral health teams end up looking for an alternative approach.
We work closely with behavioral health and treatment providers who manage admissions and insurance decisions every day.

More than 4,000 programs use our platform, with access to 1,700+ payer databases, giving us a clear view of where clearinghouses help and where intake challenges still slow teams down.
You can book a free demo today.
| Category | TriZetto | Waystar |
| Core strength | Enterprise-grade clearinghouse with strong compliance and payer connectivity | Modern, cloud-based RCM with automation and a more intuitive interface |
| Pricing approach | Fixed per-provider subscription (~$300/provider/month) | Usage-based pricing (~$0.11/claim, $0.14/eligibility) that scales with volume |
| Best fit | Large organizations prioritizing stability and predictable costs | Mid-to-large organizations focused on workflow automation and efficiency |
| Ease of use | More complex, legacy-style system with a steeper learning curve | Easier to navigate, but still requires setup and ongoing management |
| Behavioral health fit | General medical platform — limited support for intake nuance and real-time coverage decisions | Same limitation — strong for billing, but not built for admissions-first workflows |
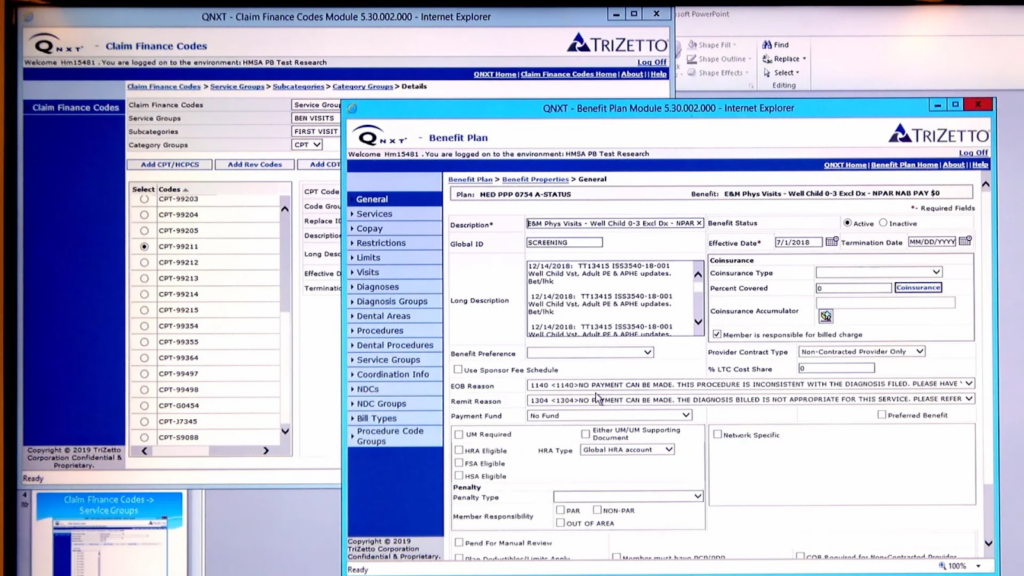
TriZetto Provider Solutions is a long-standing enterprise clearinghouse used by large healthcare organizations to process claims at scale. It supports claims submission, advanced claim edits, eligibility checks, and ERA processing, and connects to more than 8,000 payers, including Medicare, Medicaid, and major commercial plans. It also integrates with 650+ EHR and practice management systems, which is why many providers rely on it behind the scenes.
TriZetto is built for back-office billing teams. It works best when the goal is to process large claim volumes accurately and follow complex payer rules, rather than support fast intake or admissions decisions.
In practice, TriZetto fits organizations that need enterprise-grade claims processing and wide payer access. For behavioral health teams focused on quick eligibility answers during intake, it can feel heavy and removed from daily admissions work.

Waystar is a cloud-based revenue cycle platform created in 2017 from the merger of Navicure and ZirMed. It’s known for modern automation and a broad RCM feature set, handling billing for 1M+ providers and processing roughly $900B in claims annually. Waystar covers eligibility checks, claim submission and tracking, payment posting, denials, and patient cost estimates in one platform.
Waystar is built for billing and finance teams that want fewer tools and more automation. It emphasizes workflow efficiency and analytics, rather than front-door intake or specialty-specific nuance.
Waystar works best for organizations that want to centralize billing, reporting, and financial workflows in a single platform. It brings efficiency and visibility to the revenue cycle, especially for teams managing high claim volumes across multiple locations.
At a high level, TriZetto Provider Solutions and Waystar address similar billing needs, but they’re built with different priorities. For instance:
Both platforms perform well for general medical billing. Where they can fall short is timing and context.
They’re designed to process transactions after the facts are settled, not to support behavioral health admissions teams making fast calls with incomplete data, layered benefits, and payer carve-outs.
That disconnect is where delays, coverage surprises, and preventable denials tend to creep in, and why many treatment centers start looking for tools built around intake, not just billing.
Behavioral health admissions don’t follow neat, predictable paths. Calls often come in after hours, insurance details can be incomplete, and small coverage nuances can create problems later if they’re missed.
Many RCM platforms are built to process claims after information is finalized. We built VerifyTreatment to support decisions earlier, when your team is still on the phone and trying to understand coverage in real time.
If you’ve looked at general-purpose billing or clearinghouse tools and found they don’t quite fit intake workflows, here’s what makes our platform a more practical alternative for behavioral health teams.
VerifyTreatment is designed around how treatment centers actually operate. That includes residential, inpatient, PHP, and outpatient programs, along with payer rules that vary by level of care, state, and plan type.
This focus shapes how coverage information is presented. Instead of asking your team to interpret raw eligibility responses, our platform organizes benefits around treatment decisions. Admissions staff can see what applies without billing expertise, while billing and RCM teams still get the depth they need behind the scenes.

Knowing a policy is active doesn’t always tell you whether care will be covered. Many tools stop there, which leaves your team filling in the gaps.
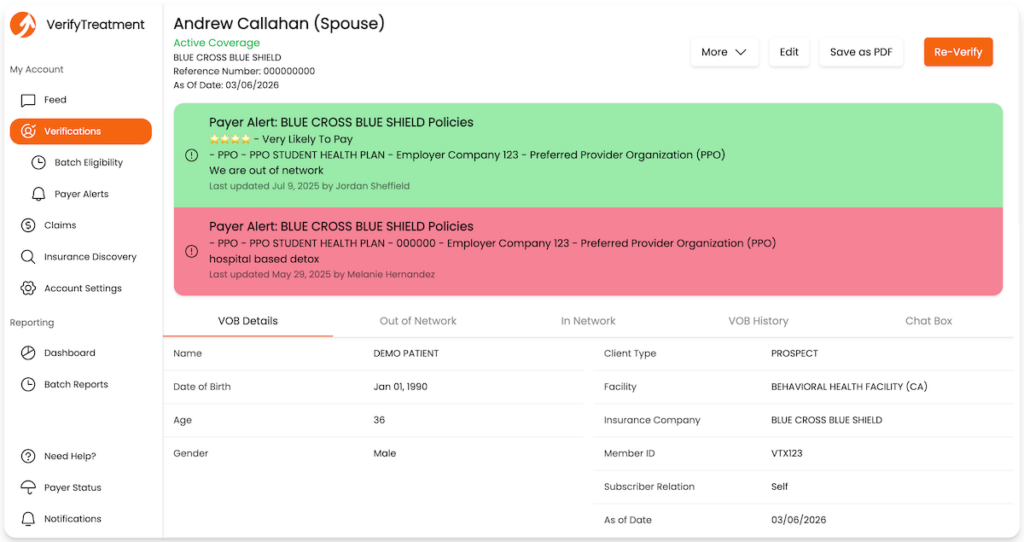
VerifyTreatment provides real-time eligibility with more payer context, so you can understand how coverage applies before moving forward.
In practice, teams may be able to review:
This helps you give clearer answers earlier, instead of sorting through surprises later in billing.
Intake calls rarely come with perfect information. Patients may not have an insurance card, may be unsure about their plan, or may be covered under a family member’s policy.
Our insurance discovery tools can sometimes identify active coverage even with limited details. For many teams, this reduces guesswork during intake and helps avoid defaulting to self-pay too quickly.
VerifyTreatment continues checking coverage after intake, giving your team earlier visibility into changes that could affect billing later on.
This can include:
For teams used to finding these issues late, this shifts some of that work earlier in the process.
The handoff between admissions and billing is often where details get lost. Information verified during intake doesn’t always carry through cleanly.
We designed VerifyTreatment to work for both teams. With Salesforce integration, verified insurance details stay connected to the patient record, so admissions and billing can work from the same information instead of re-verifying or reconciling later.
VerifyTreatment doesn’t require a long enterprise rollout. Many teams are able to get started without heavy IT involvement or drawn-out setup.
As your organization adds locations, states, or new payer mixes, verification workflows can expand without pushing your team back into spreadsheets or payer portals.
In short, teams choose VerifyTreatment because it fits how admissions actually work. It helps you get clearer coverage insight earlier, reduces back-and-forth later, and replaces manual steps with more usable information—without forcing you to adapt your workflow to a general medical billing platform.
TriZetto and Waystar are capable platforms, but behavioral health teams often need something more focused earlier in the workflow, when intake decisions are made and financial risk first shows up. VerifyTreatment is built for that front-end moment, helping teams get clearer answers sooner without adding complexity.
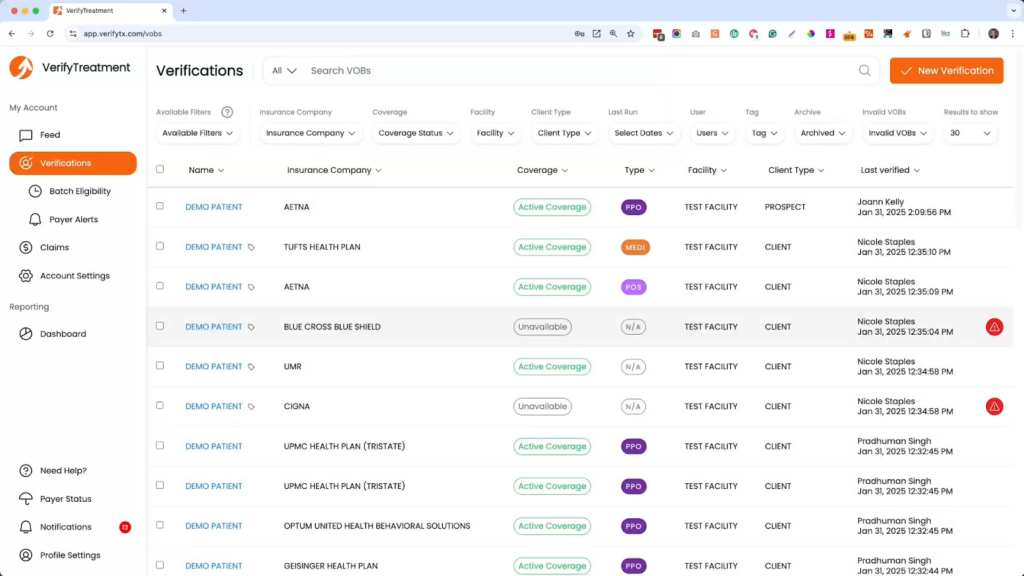
Teams often start with VerifyTreatment to:
If your team is still jumping between portals or uncovering eligibility problems after intake, it may be worth seeing a purpose-built approach in action.
A short demo of VerifyTreatment can help you decide whether it fits your workflow, without pressure and without changing how your team already works. Get started today.
Yes. Both platforms can process behavioral health claims, but they are general medical billing systems and are not designed around intake-first workflows or behavioral health–specific benefit nuance.
Waystar is usually easier to navigate thanks to a more modern interface. That said, both tools are still built for billing teams rather than fast-moving admissions workflows.
TriZetto typically uses flat, per-provider monthly pricing. Waystar often uses transaction-based fees, which can rise as claim or eligibility volume increases.
Not especially. Both generally expect accurate policy details up front, which can be difficult during real-world intake calls.
VerifyTreatment is often chosen because it’s built specifically for treatment centers, with deeper eligibility detail, insurance discovery, and workflows designed around admissions rather than back-end billing.
Many teams start by looking at how often eligibility issues delay intake or surface later as denials. If that’s a recurring problem, a short demo is usually enough to see whether it fits their workflow.
Disclaimer: All trademarks, logos, and brand names are the property of their respective owners. The use of any third-party trademarks, logos, or brand names in this article is for informational and comparative purposes only, and constitutes nominative fair use. This article was published by VerifyTreatment, and while we strive for objective comparisons, VerifyTreatment is included as an option within this list.




Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.