
This VerifyTreatment guide highlights the top behavioral health tools across key categories, including insurance verification, EHR/practice management, billing, and prior authorization. Below is a shortlist of leading options in each category, followed by a comparison table.
| Tool | Category | Best for |
|---|---|---|
| VerifyTreatment | Insurance Verification & Eligibility | Real-time eligibility, insurance discovery, lapse detection built for behavioral health. |
| TherapyNotes | Practice Management & EHR | Simple, BH-focused EHR with notes, scheduling, billing and telehealth. |
| Cantata Health (Arize) | Billing & RCM | Deep RCM automation and denial prevention across sites. |
| Waystar | Claims Management | Enterprise clearinghouse + smart edits to cut denials at scale. |
| Myndshft | Prior Authorization | Automated PA + eligibility orchestration to speed approvals. |
Many behavioral health programs spend too much time on manual tasks. Slow coverage checks, payer portals, and billing issues can hold up intake and add extra work for clinical and admin teams.
Modern behavioral health software eases that load by cutting manual steps and giving teams accurate information early in the process.
This guide highlights leading options across key categories, with a focus on tools built for behavioral health.
VerifyTreatment works in behavioral health RCM every day. Our real-time verification and RCM platform was built by people with years of experience in admissions, billing, and payer-facing roles. Today, thousands of treatment centers use it, including more than 4,000 providers who run benefit checks through our system.
“Great Product, Ease of Use, Added Efficiency for Our Team. Automating and bringing in health insurance verifications to our instance was a game changer. We have instant verifications for all of our prospects, as well as automated verifications for our clients on a weekly basis.”

“The product is lightning fast, and so easy to use. In terms of instant verification, there is nothing faster or more comprehensive in my experience. Highly recommend for billing and admissions departments.”

We see what slows intake and what creates billing problems, and we’ve seen how the right software can fix those issues. That experience shaped this list, giving you a clear view of which tools may fit your workflow.
You can book a free demo today.
Here’s a simple comparison table to help you see the differences at a glance.
| Product | Category | Key features | Pricing | Best for |
|---|---|---|---|---|
| VerifyTreatment | Insurance Verification & RCM | Real-time eligibility, insurance discovery, lapse detection, ERA/claim tracking, Salesforce integration | Custom quote | Behavioral-health treatment centers |
| InstantVOB | Insurance Verification | Instant VOB, co-pay/deductible details, mobile access, tiered VOB packs, API option | $179.99/mo (50 VOBs) or $149.99/mo billed annually | After-hours intake & mid-volume clinics |
| pVerify | Verification & Data Services | Eligibility, insurance discovery, MBI lookup, claim status, batch/API workflows | Starting tiers $40–$125+ per module | Multi-payer, multi-state clinics |
| TherapyNotes | Practice Mgmt & EHR | Note templates, scheduling, billing, telehealth, add-on eligibility | Solo $69/mo; Group $79 + $50/addl clinician | Solo therapists, small clinics |
| SimplePractice | Practice Mgmt & EHR | Tiered plans, telehealth, client portal, claims handling, intake forms | Starter $49 / Essential $79 / Plus $99 per mo | Solo to small group practices |
| Valant | Practice Mgmt & EHR | BH-first EHR, outcomes tracking, billing, multi-role dashboards, integrations | Custom quote | Growing BH clinics & groups |
| Cantata Health (Arize) | Billing & RCM | Claims cleaning, denial prevention, A/R dashboards, workflow rules, analytics | Custom quote | Medium→large BH orgs |
| Qualifacts | EHR & BH Platform | ONC-certified EHR, billing, reporting, compliance modules, integrations | Contract / custom | Large agencies and networks |
| BehaveHealth | BH Platform (EHR+RCM) | CRM + EHR + RCM + ERP, denials, UR, patient financials, training | Custom quote | Multi-program treatment providers |
| Waystar | Claims Management / RCM | Eligibility automation, intelligent edits, payer connectivity, coverage detection | Custom quote | Enterprise RCM teams |
| Availity Essentials Pro | Clearinghouse / Claims | All-payer hub, eligibility, PA support, claim status, analytics | Custom / contact sales | Clinics needing broad payer reach |
| Myndshft | Prior Authorization & Eligibility | Real-time PA automation, eligibility, COB, rules engine, cost calc | Custom quote | PA-heavy clinics and hospitals |
| Surescripts ePA | ePA (pharmacy) | Electronic PA, dynamic question sets, PBM connectivity, EHR integrations | Free portal for prescribers (integration fees vary) | Clinics needing faster medication PAs |
Behavioral health programs need quick insurance checks to keep admissions moving. The tools below give teams clear coverage information right away.

VerifyTreatment is built specifically for behavioral health, so it handles the coverage issues that slow down intake in treatment centers. Programs that switch to our platform often report quicker admissions, fewer eligibility problems, and a clear drop in denials linked to missing benefit details.
Most verification tools are made for broad medical use. VerifyTreatment focuses on behavioral health from the start, which means it reads complex Medicaid plans, multi-state policies, and payer rules that often confuse other systems.

Instead of returning a basic “active/inactive” result, the platform shows full benefit details in seconds, even when patient information is limited. The platform also flags inactive policies, tracks claim status, shows patient responsibility, and alerts staff when coverage data changes.

In short, VerifyTreatment gives your team the speed and clarity needed to make informed decisions on the first call and keep revenue on track.
Tailored pricing with a 30-day money-back option.


InstantVOB is a simple, web-based tool for quick insurance checks at any time. It supports a wide range of payers, including many mental health and substance use plans.
Staff enter basic patient details into an online form, and the platform returns coverage information within seconds. This helps admissions teams confirm core benefits without logging into payer portals or waiting for business hours.
Because the system is fully cloud-based, teams can use it on desktops, tablets, or mobile devices. Many treatment programs use it as a backup or overflow option when they need a fast way to confirm active status, deductibles, co-pays, and other basic benefit details.


pVerify is a long-running eligibility and claims tool used across medical, dental, vision, and behavioral health settings.
It supports real-time checks with wide payer coverage and returns detailed benefits in one lookup. Teams can see active status, deductibles, co-pays, authorization needs, and out-of-pocket limits without moving through several portals.

Practice management/EHR systems combine clinical record-keeping with office management. In behavioral health, these are the top solutions
TherapyNotes is a widely used behavioral health EHR for therapists, counselors, and small group practices. It brings scheduling, notes, billing, and client communication into one system, which helps reduce the time staff spend moving between different tools. Users often highlight its clear layout and steady performance, making day-to-day work easier.
The platform includes built-in telehealth, secure messaging, and a billing module that can submit claims, track EOBs, and run eligibility checks in real time. This helps small practices cut down on rejected claims and keep clinical and billing tasks aligned.

SimplePractice is a cloud-based practice management system for therapists and counselors that brings scheduling, billing, documentation, and telehealth into one place. It’s built for solo and group practices that want a clear layout, quick setup, and features that fit everyday outpatient work.

Valant is a cloud-based EHR built specifically for behavioral health. It supports practices of many sizes and brings scheduling, documentation, billing, and patient engagement into one platform. Its large library of therapy-focused templates helps clinicians complete notes quickly and keep documentation consistent.

One standout feature is Valant’s support for measurement-based care. The system tracks outcome scores automatically, giving teams a clear view of patient progress through structured tools.
Behavioral health programs need solid RCM tools to keep claims moving and avoid lost revenue. Below are RCM platforms built to support behavioral health workflows:
Cantata Health’s Arize platform is an EHR and RCM system built for health and human service organizations. The RCM module brings eligibility checks, claims work, and payment management into one system, which helps billing teams support multiple programs or locations from a central office.
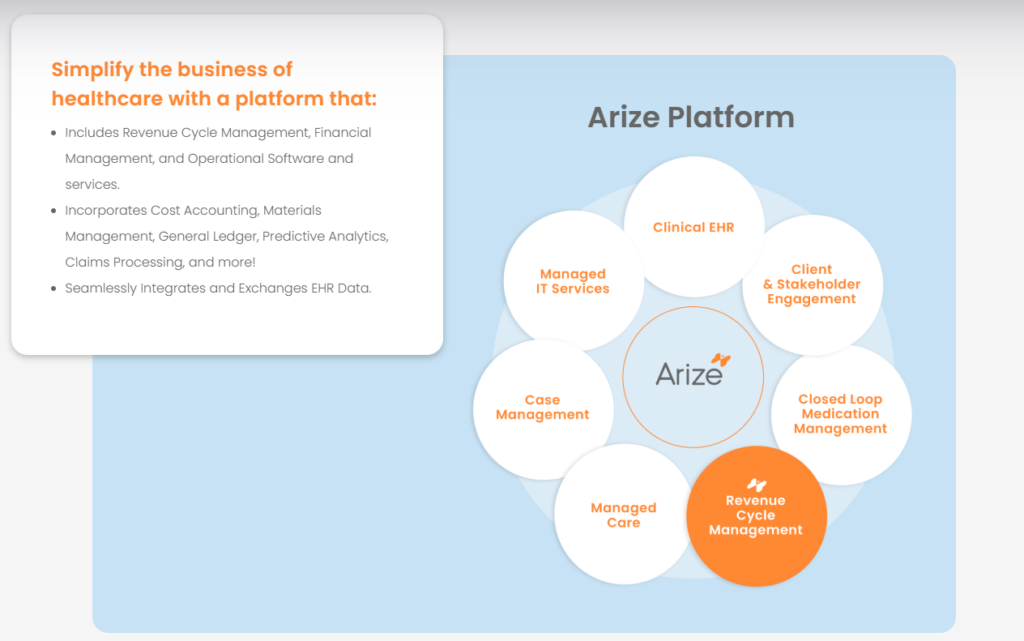
Arize focuses on keeping claims clean before they reach the payer. Built-in rules help staff spot common issues early, and its accounting tools support organizations that manage payments across several sites.
Not published. Requires direct contact with the vendor.
Qualifacts offers EHR platforms (CareLogic and Credible) with RCM built into the same system. Many agencies use it because clinical notes, scheduling, billing, and reporting all run in one workflow, which reduces delays that happen when teams jump between several tools.

The platform supports eligibility checks, claims editing, payment posting, and patient statements. Some organizations also use Qualifacts’ outsourced billing service for follow-up and call-center support.
Not published. Demo required to receive a quote.
BehaveHealth is an all-in-one platform built for addiction treatment programs. Its RCM system covers the full billing cycle, giving teams tools to verify coverage, manage authorizations, submit claims, and track denials in one workflow.

Because the RCM module connects directly with admissions and clinical records, staff can move information across departments without re-entering details. The VOB tool checks eligibility and detailed benefits and stores the results in the patient record, helping admissions confirm coverage before treatment begins.
The platform also supports utilization review by matching clinical information with payer rules. Claims, remits, and appeals stay in a single system, which helps billing teams stay organized.
Not published. Contact required for details.
Claims management tools help improve claim accuracy and speed up payments. They apply edits, attach required documents, and give teams a simple way to manage rejections and follow-ups. Below are leading clearinghouse options used in behavioral health.
Waystar Claim Manager is a clearinghouse tool that helps billing teams submit cleaner claims with less manual work. It connects to many EHR and practice-management systems, so teams can review claims, fixes, and payer responses in one place.

The platform applies automated edits before submission and uses an AI-supported rule engine to catch issues that often lead to rejections. This helps high-volume billing teams prepare claims more accurately and reduce delays.
Quote-based (requires a sales call).
Availity Essentials Pro expands on the company’s long-standing payer portal by offering a complete RCM workflow. It brings eligibility checks, authorizations, claim edits, claim status, and remittance posting into one system, allowing billing teams to move through each stage with fewer handoffs and less manual tracking.

The system analyzes claims with predictive edits before submission, which can help staff spot missing or incorrect details earlier. It also links authorization steps to the claim workflow, giving billing teams quicker access to required information.
Quote-based (contact Availity for details).
Prior authorization tools help behavioral health programs get treatment and medication approvals without long delays. Many psychiatric medications and certain therapy services require payer sign-off, which can slow intake and disrupt care.
PA platforms cut that manual work by automating forms, pulling clinical details, and tracking responses in one place. Below are two leading options.
Myndshft includes a combined medical and pharmacy PA workflow. The platform supports fast submissions by pulling plan information, filling required fields, and sending requests through the correct medical or pharmacy channels.

For behavioral health programs, this can give prescribers a clearer path to approval during or shortly after a patient visit.
The system handles form population, status updates, and appeal steps in one place. This helps staff avoid repeated phone calls, manual form checks, or switching between portals.
You need to get a custom quote.
Surescripts powers one of the largest e-prescribing networks in the country, including a nationwide system for electronic prior authorizations on medications. It connects directly with many EHRs, pharmacies, and health plans, allowing clinicians to complete drug PAs without leaving their normal prescribing workflow.

The system sends PA requests, receives decisions, and updates the provider in real time. This helps patients start medications sooner and reduces the back-and-forth that slows care. For teams without EHR integration, Surescripts also offers a free web portal for submitting ePAs online.
Quote required (pricing available after contacting Surescripts).
Insurance verification only works if it’s fast, accurate, and reliable. Every tool on this list can help, but if you run a behavioral health program with high volume, complex payers, or frequent eligibility issues, VerifyTreatment is built for exactly that reality.
You can trust us for real-time benefits, deep payer logic, insurance discovery, and lapse alerts, all built to keep admissions and billing running smoothly. Thousands of treatment centers rely on us to avoid coverage surprises and reduce eligibility-related denials.
Book a quick demo with VerifyTreatment today.
It’s software built for mental health and SUD programs, including EHRs, practice-management systems, eligibility tools, billing platforms, claims managers, and PA solutions.
BH software handles Medicaid carve-outs, managed-care rules, clinical needs, and SUD workflows that general medical systems often miss.
Start with your biggest problem, like slow intake, documentation gaps, eligibility issues, or denials, and choose the tool built to solve it.
Not usually. Most behavioral health platforms offer guided onboarding and phased rollout so teams can keep working without major interruptions.
VerifyTreatment gives real-time eligibility, deep payer logic, insurance discovery, lapse alerts, and full benefit detail made specifically for BH programs.
Yes. It supports unlimited users, batch verification, CRM/EHR integrations, and payer coverage across states.
No. Most BH platforms, including VerifyTreatment, are designed for non-technical staff with simple, clear workflows.
Disclaimer: All trademarks, logos, and brand names are the property of their respective owners. The use of any third-party trademarks, logos, or brand names in this article is for informational and comparative purposes only, and constitutes nominative fair use. This article was published by VerifyTreatment, and while we strive for objective comparisons, VerifyTreatment is included as an option within this list.



Samantha is a dynamic marketing professional dedicated to making a difference in the behavioral health industry through her work at VerifyTreatment. With a strong background in digital marketing and brand advocacy, she helps elevate the platform’s presence by fostering authentic connections with treatment centers and healthcare providers. Her expertise in content creation and community engagement ensures that VerifyTreatment’s value is communicated effectively, helping centers streamline operations and improve patient care. Samantha’s focus on building trust and driving awareness positions VerifyTreatment as a key resource in the healthcare landscape.

Nicole is a versatile healthcare professional with a Bachelor’s degree in Health Administration and a solid background in managing healthcare systems and operations. Her experience spans healthcare management, compliance, and regulations, making her adept at navigating complex healthcare environments. In addition to her administrative expertise, Nicole holds certifications in Functional Nutrition and Personal Training, giving her a well-rounded perspective on health and wellness. She is committed to using her skills to improve healthcare settings and ensure effective, patient-centered care.

Tara is a dedicated leader who leverages her Master's degree in Information Technology (Florida Tech) and deep company knowledge (since 2018) to drive our community awareness. She is the central figure for managing social engagement and ensuring the community is immediately and effectively informed of all new product launches and company updates.

JoAnn has a strong background in the mental health and substance abuse industry, with expertise in billing, coding, facility credentialing, and contracting. She is passionate about team education and public speaking, always striving to make a positive impact. With a solid foundation in accounting, JoAnn also holds an Associate of Arts in Biblical Studies from Liberty University, blending her professional skills with her personal values.

For 11+ years, Melanie has been dedicated to helping clients access quality mental health care, with a special focus on grief, loss, and substance abuse. With expertise in healthcare, community outreach, patient advocacy, and leadership development, Melanie is passionate about making a positive impact in the lives of others.

Jordan is a dedicated advocate for behavioral health and is passionate about improving sales strategies and business processes. With a focus on helping businesses, particularly in healthcare, Jordan believes that streamlining operations is a way to positively impact more people indirectly. A strong leader, both personally and professionally, Jordan is committed to making a difference in the world by doing good business and serving a higher purpose.